Tag
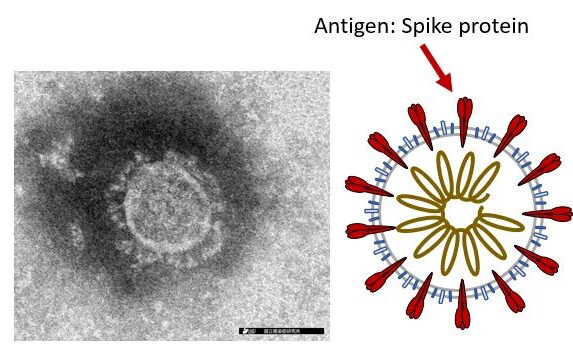
COVID-19
-
How to use health equity data to cover access to COVID‑19 rapid tests
When the Biden Administration rolled out two COVID-19 rapid tests programs in mid-January, Kaiser Health News reporters Victoria Knight and…

-
Omicron subvariants “of concern” drive surge in cases and reinfection rates
The COVID-19 story of the summer is omicron subvariants. As of mid-July, two subvariants are “of concern,” according to the…

-
Advocates, hospitals at odds about CMS plan to suppress a patient-safety score
Federal officials intend to give hospitals a break in quality scoring due to pandemic strains, by halting reporting of a…

-
Expert insight and resources for covering Paxlovid and other COVID-19 treatments
In December 2021, Pfizer announced the significantly positive study results of its COVID-19 antiviral Paxlovid. The study enrolled unvaccinated people at high-risk…

-
A closer glance at long COVID: What to know
Long COVID, long haulers, post-COVID syndrome, post-acute sequelae of COVID — from the early days of the pandemic — there…

-
Resources for covering mysterious hepatitis in kids
Hundreds of young children in the U.S. and the United Kingdom have developed hepatitis — inflammation of the liver —…

-
Former CDC leaders say agency needs more funding and better communication to restore trust
Former directors of the Centers for Disease Control and Prevention gathered for an online debate last week to discuss ways to…

-
Resources for reporting on COVID-19’s origins
Since the early months of 2020, scientific debate has raged over the origin of COVID-19 and whether it emerged from…

-
What AHCJ is doing to make HJ22 safe (and well worth the trip)
With just a few days left before early-bird registration ends, AHCJ’s staff have been finalizing conference planning at Health Journalism…