Tag
HIV
-
Caution and ideas for covering HIV/AIDS in 2019
In April 1984, then-U.S. Health and Human Services Secretary Margaret Heckler announced the National Cancer Institute had discovered the virus…

-
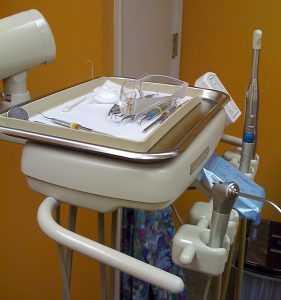
Investigations put focus on infection control in dental offices
Two high-profile safety breaches have highlighted the importance of close adherence to infection control protocols in dental clinics and offices.…

-
Advice from a reporter experienced in interviewing people in stigmatized populations
Heather Boerner’s October 2018 piece at NPR examined the fate of people who live without treatment for their HIV after…

-
Connecting the dots between social determinants and infectious diseases
Socioeconomic factors such as poverty and living conditions play a role in shaping infection risk and disease outcomes. Many times…

-
Infectious disease outbreaks rise with opioid epidemic
Cases of infectious diseases such as hepatitis A, B and C, sexually transmitted diseases (STDs) and human immunodeficiency virus (HIV)…

-
Covering HIV in the modern era: What reporters need to know
About 36.7 million people around the world – about 1.1 million in the U.S.- are living with an HIV (human…

-
Tips to expand coverage of LGBT health beyond HIV and AIDS
For the past several decades, HIV and AIDS have dominated discussions and reporting about LGBT health. While HIV/AIDS continues to…

-
Resources for covering HIV/AIDS in the aging population
Thanks to a variety of antiretroviral medications available, especially the widely used HAART combination therapy, those who contracted HIV/AIDS from…

-
Health insurance discrimination persists for those with HIV, cancer and other conditions, despite ACA
Over the past two years, patient advocacy groups, researchers and consultants have said health insurers have discriminated against their members…

-
•
Despite progress fighting HIV, most vulnerable still at risk #ahcj15
HIV prevention and treatment have undergone a revolution since the disease first appeared, but there are still barriers to reaching…