Tag
HIV
-
Why HIV funding cuts would impact every community
Major funding cuts to HIV and AIDS services could lead to a loss of viral suppression in current patients and…

-
Redlining’s lingering public health legacy
Recent studies show that people from formerly redlined neighborhoods face multiple health disparities including a lower life expectancy.

-
Trump’s data purge: What to know about federal infectious disease sites
It’s unclear how much we can rely on the CDC for ongoing, reliable data after more than 1,000 pages with…

-
Opportunities to localize coverage from International AIDS Conference
New advances in HIV PrEP, prevention and viral suppression at AIDS 2024 Conference can translate to local story ideas.

-
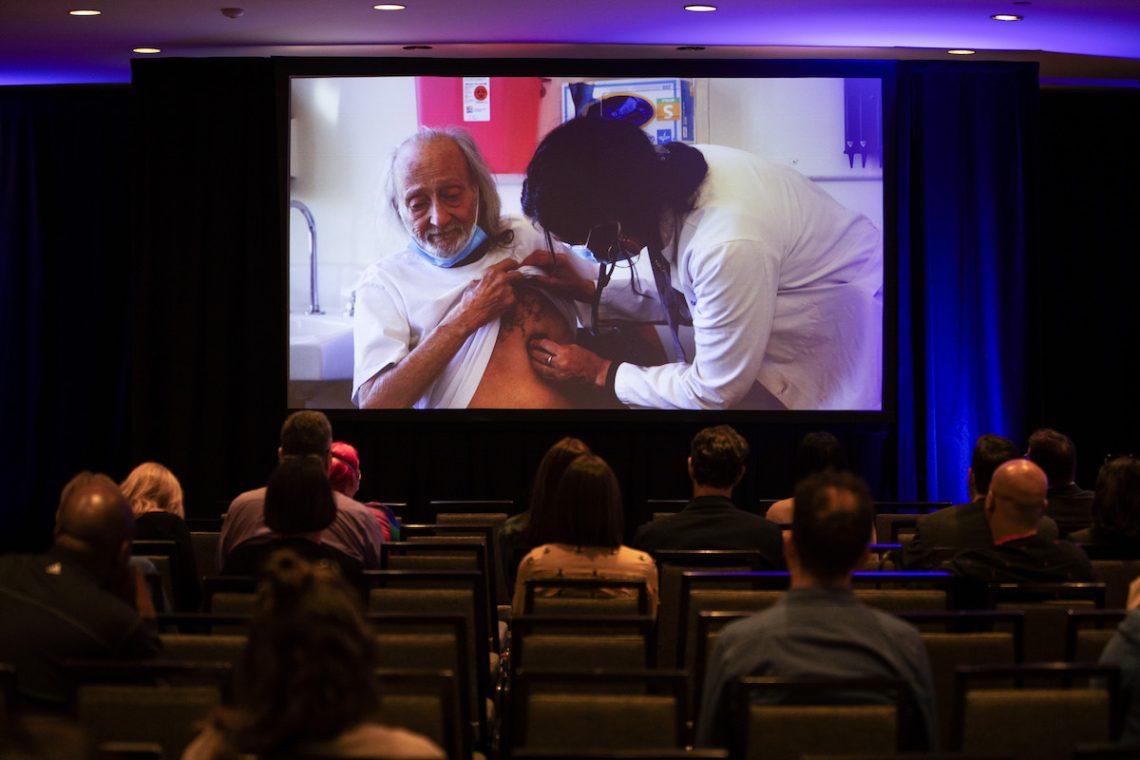
HIV treatments stem transmission, but stigma, barriers to access persist
Following a screening of “Ending HIV in America” at HJ24, panelists discussed why it’s still difficult to make treatments widely…

-
Why this matters: HIV, TB conference offers wealth of story ideas, sources
Learn how to identify feature story ideas and second-day stories from an infectious disease conference focused on HIV and tuberculosis.

-
Reporting on disparities in HIV testing, PrEP
HIV trends don’t make headlines the way they used to. But we may see an influx of them in the…

-
Covering HIV angles and updated HIV and AIDS resources tip sheet
Most of our attention over the past year has been on the COVID-19 pandemic, but AIDS (acquired immunodeficiency syndrome) and…

-
Infectious disease rates rising with opioid epidemic
As the opioid crisis has continued to plague the nation, a less-reported story for journalists to consider is the surging…

-
Report details unmet needs of older adults living with HIV/AIDS
At the beginning of the AIDS epidemic in the 1980s, those with the disease typically only lived a few years…