Tag
costs
-
Medicare announces coverage of costly Alzheimer’s medication. That could mean high premiums for beneficiaries
Medicare coverage of new Alzheimer’s treatments will raise premiums and increase out-of-pocket costs for beneficiaries, new analysis finds.

-
Teeth have an expiration date
In the next few months, what I’ll be spending on fixing my teeth will eat up much of what I’ll…

-
Does care suffer as private equity firms buy struggling nursing homes?
Private equity firms are in the business of making money. On the surface, there is nothing wrong with that. However,…

-
Experts have advice for the last-minute Medicare Advantage shoppers among your audience
Watching the TV ads during the evening news, you would think Medicare Advantage plans were the greatest health insurance bargain…

-
Employers and insurers paid hospitals 247% more than Medicare rates, new study shows
Research released today shows that from 2016 through 2018, self-insured employers and commercial health insurers in 49 states and the…

-
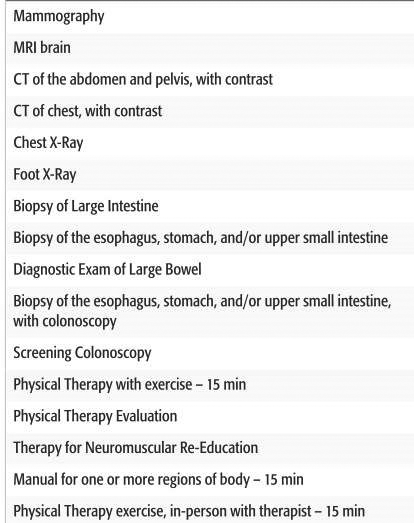
Wide variations in health care providers’ charges raise questions about the right rate
Early last month, a report from the Pioneer Institute in Boston showed that Massachusetts consumers could have saved $22 million…

-
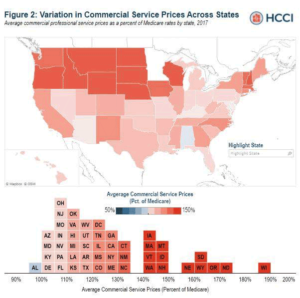
Report shows wide variation in what insurers pay providers versus what Medicare would have paid
During the coronavirus pandemic, any number of good news stories seem to get little or no coverage because most health…

-
Even in a pandemic, it’s important to keep the price transparency issue in perspective
A federal judge last month ruled against the American Hospital Association and other hospital groups in their lawsuit against the…

-
Reporter explores impact of medical credit cards on dental debt
Dental patients in need of costly procedures may turn to medical credit cards to pay for the services. But these…

-
Scrutiny of hospital charges likely to intensify in wake of pandemic
As the nation’s hospitals strain to keep up with the demand to care for COVID-19 patients, it seems almost unfair…