Early last month, a report from the Pioneer Institute in Boston showed that Massachusetts consumers could have saved $22 million in 2015 if they got health care from lower-cost providers instead of from the highest-priced health care providers.
In “Analysis of Spending on Shoppable Services in Massachusetts,” researchers wrote that consumers could have saved $116.6 million if the savings were adjusted for inflation over four years.
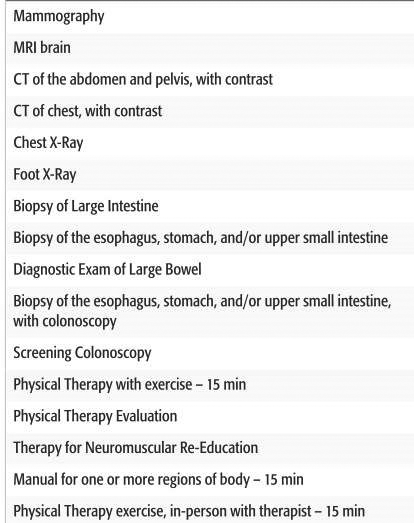
The researchers analyzed what providers charged in 2015 for 16 shoppable services, such as elective or non-emergent surgery.
Wide variations in what hospitals, health systems, physicians and other providers charge are not news. As many health care journalists know, such differences in provider charges are common nationwide. We recently covered another report on this topic.
Researchers from the Health Care Cost Institute, in “Comparing Commercial and Medicare Professional Service Prices,” recently compared what health insurers paid to physicians and other providers with what Medicare pays for those services. On average, what health insurers paid for professional health care services was 122 percent higher than what Medicare paid in 2017, according to researchers, who also found that average commercial prices varied widely from one state to another.
What these two reports, and dozens of others like them, show is that the nation’s fragmented health care system allows hospitals, physicians, and other providers to charge whatever the market in their cities and towns will bear.
Earlier this year, the federal Centers for Medicare and Medicaid Services (CMS) issued a rule requiring hospitals to release pricing information before providing services. The rule, which is not yet in effect due to pending litigation, would require hospitals to list standard prices for 300 shoppable services and the lowest rates they would accept when consumers pay out of pocket.
“According to CMS Administrator Seema Verma, the new price transparency rule will help patients by boosting quality and cutting costs,” according to researchers who wrote about the new CMS rule in Health Affairs last spring.
It’s debatable whether price transparency will help improve quality and cut costs, as Verma suggests. Consumers are like others who buy health care in that they want value, which we can define as the best quality at the lowest price. The search for value is at the heart of what health care experts call value-based care, a topic we’ve covered extensively in the past few years.
In a new AHCJ tip sheet, we explore the relationship between value-based care and what is the right rate. We also show how the pursuit of value-based care has roots that go back to at least the 1970s and the pursuit of what is the best rate.




