During the coronavirus pandemic, any number of good news stories seem to get little or no coverage because most health care journalists are busy covering COVID-19.
One such case in point was a report earlier this month from the Health Care Cost Institute. In Comparing Commercial and Medicare Professional Service Prices, HCCI researchers compared what health insurers paid to physicians and other providers with what Medicare pays for those services.
This report should not be overlooked for at least three reasons. First, the research is useful for health care journalists writing about how much physicians and other providers are paid for professional clinical services in their states versus a national benchmark such as Medicare rates. The report includes an interactive map showing the variation between what health insurers paid and what Medicare paid.
Second, the report shows a wide variation in what physicians and other providers are paid versus what Medicare would have paid. Wide variation in prices is not a new topic, of course, but whenever it comes up, a valid question worth is why are charges so high in some states and much lower in other states.
Third, the report adds context to the debate over what hospitals charge versus Medicare rates, which is a topic we’ve covered extensively in recent months, including this blog post in April.
The HCCI researchers showed that from 2014 to 2018, what physicians and other providers were paid for health care services accounted for about 75% of the increase in health care spending above inflation. Earlier this year, Adam Cancryn reported for Politico on a Politico-Harvard poll showing that health care costs were a top concern among Americans, at least pre-pandemic. Therefore, what physicians and other providers are paid may inform reporting on health policy during this election cycle, when Medicare for All will be widely debated.
The HCCI study reviewed 210 million claims from individuals who had health insurance through their employers in 2017. After calculating the average commercial prices paid for 500 common professional services in 271 metropolitan areas in 48 states and Washington, D.C., they compared the prices paid for those services with what Medicare would have paid for the same services under Medicare’s physician fee schedule.
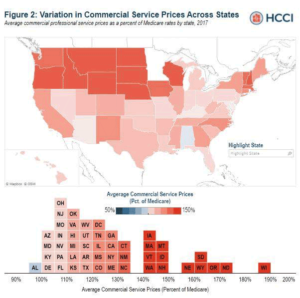
“We find that commercial prices for professional services were, on average, 122 percent of Medicare rates nationally in 2017,” the researchers wrote. “Average commercial prices varied dramatically across states, from below Medicare rates in Alabama (98 percent of Medicare) to nearly twice Medicare rates in Wisconsin (188 percent of Medicare).”
Also, they found variation in how commercial prices compared to Medicare rates within states. In California, for instance, commercial prices averaged 95% of Medicare in Bakersfield but 178% of Medicare in Santa Cruz. In other states, commercial prices were similar among metropolitan areas, ranging from 107% to 120% above Medicare rates in Louisiana, for example.
“The variation we find both across and within localities suggests that any policies that rely on benchmarking commercial prices to Medicare rates may have a dramatically different impact depending on the area,” the researchers explained. “For example, a policy capping commercial rates for out-of-network providers at 150 percent of Medicare would lower rates paid to providers in Bakersfield on average, while increasing rates paid to providers in Santa Cruz.”
In no state did the average commercial health insurance rates paid to physicians and other providers exceed 200% of what Medicare paid. But the report showed that in five areas in Wisconsin ― LaCrosse-Onalaska, Eau Claire, Marinette, Green Bay, and Sheboygan ― insurers paid more than 200% of what Medicare paid. In Alabama, what insurers paid was below what Medicare paid in 23 metropolitan areas.




