Tag
prices
-
Tariffs and meds: What health journalists should watch for now
The story of tariffs on medications has shifted quickly in recent weeks due to new trade agreements, industry reactions and…

-
How rising health care prices are harming employers and families
In this webinar, learn about the rising spiral of health care prices and the impact it’s having on employers and…

-
Wide variations in health care providers’ charges raise questions about the right rate
Early last month, a report from the Pioneer Institute in Boston showed that Massachusetts consumers could have saved $22 million…

-
Report shows wide variation in what insurers pay providers versus what Medicare would have paid
During the coronavirus pandemic, any number of good news stories seem to get little or no coverage because most health…

-
Scrutiny of hospital charges likely to intensify in wake of pandemic
As the nation’s hospitals strain to keep up with the demand to care for COVID-19 patients, it seems almost unfair…

-
GAO report confirms the financially toxic nature of air ambulance fees
Over the past several years, health care journalists have done great work highlighting the problem of surprise medical bills. There’s…

-
Series on pharmacy benefit managers makes complicated topic easier to understand
One of the most complicated topics to cover in health care today is the role of pharmacy benefit managers (PBMs).…

-
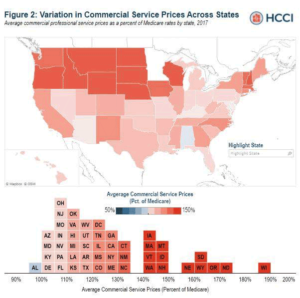
New report finds wide variation in health care costs among states
Consumers in states with high health care costs spend more than twice as much for certain services than consumers in…

-
Six (or more) things to remember when reporting on health care costs
Health care costs lack transparency and are wildly variable, not just from region to region but sometimes from block to…