Tag
Congress
-
Telehealth for Medicare beneficiaries gets another reprieve
The continuing resolution avoiding a government shutdown also extended telehealth benefits for Medicare beneficiaries for six months.

-
Older Americans Act reauthorization in limbo: What to know
Reauthorization of the Older Americans Act, which provides vital services to millions of people 60 and older, might be on…

-
History shows Inflation Reduction Act subsidies help Americans save on health insurance
By signing the Inflation Reduction Act (IRA) on Tuesday, August 16, President Biden made history by continuing a 12-year trend…

-
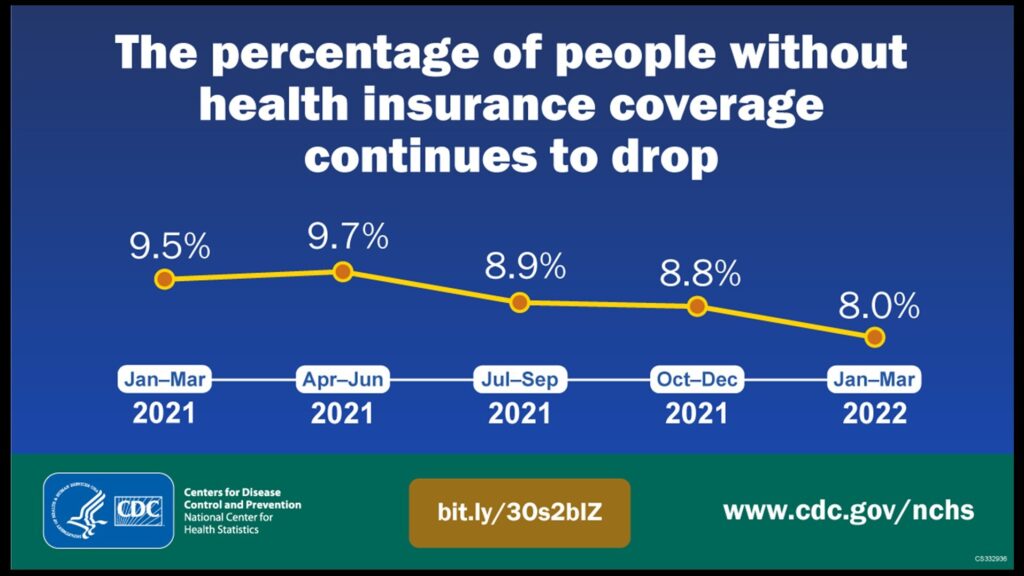
3 reasons it’s significant that the percentage of uninsured Americans hit an all-time low
The percentage of Americans who lack health insurance hit an all-time low of 8% in the first quarter of this…

-
Fixing the public health system for the next pandemic
The American Rescue Plan (ARP), passed by Congress last month, will be sending about $100 billion into the U.S. public…

-
Congress strikes taxes that helped pay for the ACA
Remember all those taxes and fees meant to pay for the Affordable Care Act? The ones that keep getting delayed,…

-
Congress watch: Why Medicare coverage of unmet needs is so vital
Congress returns from its summer recess with a full agenda. It’s probably not high on its to-do list, but many…

-
New law signed aims to better target Alzheimer’s prevention, treatment
Despite the partial government shutdown, some wheels in Congress keep turning. Among them, the BOLD Act (Building Our Largest Dementia…

-
With elections behind us, what to expect for the Health Policy landscape
The midterm election and a divided Congress creates a new Health Policy agenda for 2019. Repeal is done – in…

-
Congressional inaction leaves states squeezed on CHIP funding
With Congress failing to meet a Sept. 30 deadline to extend federal funding, the Children’s Health Insurance Program (CHIP) now…