Tag
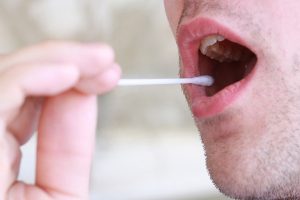
testing
-
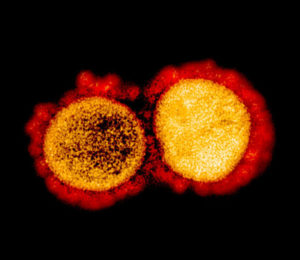
Reporter looks at misuse of rapid COVID-19 tests in nursing homes
It can be difficult in normal times to get reliable, timely information from many long-term care facilities without filing FOIAs…

-
As death rates rise, nursing and LTC facilities face critical testing, PPE challenges
Six months after the first nursing home residents died of the novel coronavirus, many nursing homes and long-term care facilities…

-
Local officials on watch for unauthorized COVID-19 test sites
Cities, counties and states around the country are probably on heightened alert for unauthorized pop-up COVID-19 testing operations after San…

-
AHCJ webcast to feature Harvard pathologist on coronavirus testing
As the number of SARS-CoV-2 infections and deaths due to the COVID-19 disease increase daily nationwide, journalists are asking why…

-
Congress, regulators offer financial relief for Americans seeking tests, treatment for new coronavirus
The just-passed multibillion-dollar Families First Coronavirus Response Act includes free diagnostic testing for the new COVID-19 illness — for those…

-
Story about genetic testing company’s problems shows how good reporting stands up to criticism
In December 2016, Charles Piller (@cpiller), the west coast editor for Stat, reported that a genetic test to identify patients…

-
False positives matter: A real-life case study in understanding context
Something happened in our family early in August that set me behind in my work for more than three months.…

-
AHCJ award winner spoke at professional meeting of industry she investigated
Last fall, I was fortunate to hear journalist Ellen Gabler give a presentation about one of her investigations to a…

-
When patients get lab test results, journalists may need these resources
Next month, all clinical laboratories must make patients’ laboratory test results available to patients who request them. Under rules three…

-
•
Patients at risk after free public screening
UPDATE: Commenter CT points out that the students involved were not medical school students but were in the University of…