Tag
hhs
-
ACIP meeting countdown: COVID vaccine and what else is at stake
In this webinar, panelists discussed a federal judge’s breaking news ruling to halt multiple vaccine decisions made by RFK and…

-
Federal judge halts HHS, ACIP vaccine decisions: What to know
On Monday, a federal court temporarily blocked multiple decisions made by HHS and its vaccine advisory panel since May 2025.…

-
•
Vaccine injury compensation in the U.S.: Current practices and future prospects
In this webinar, hear from the Expert Vaccine Analysis Team about potential big changes to the federal Vaccine Injury Compensation…

-
The latest on the harms of private equity in health care
Three reports have been issued in January on the harms of private equity in health care. Journalists should keep up…

-
Kennedy’s hearings for HHS Secretary start today: What Americans need to know
As Robert F. Kennedy Jr.’s confirmation hearings begin, journalists can report on recent developments about his anti-vaccine views and disregard…

-
Understanding RFK Jr.’s potential HHS powers and why to avoid ‘sane-washing’ him
It’s crucial for your audience to understand how dangerous Robert F. Kennedy’s beliefs are to public health.

-
•
What Kennedy could do: Reporting on U.S. vaccine policy and the powers of the HHS Secretary
This webinar will cover the ins and outs of vaccine policy and what Kennedy could do if approved as HHS…

-
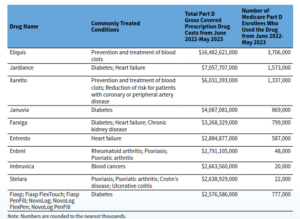
HHS names first 10 drugs for price negotiations under the Inflation Reduction Act
The Biden administration named the first 10 prescription drugs on Tuesday that will undergo Medicare price negotiations starting this year.…

-
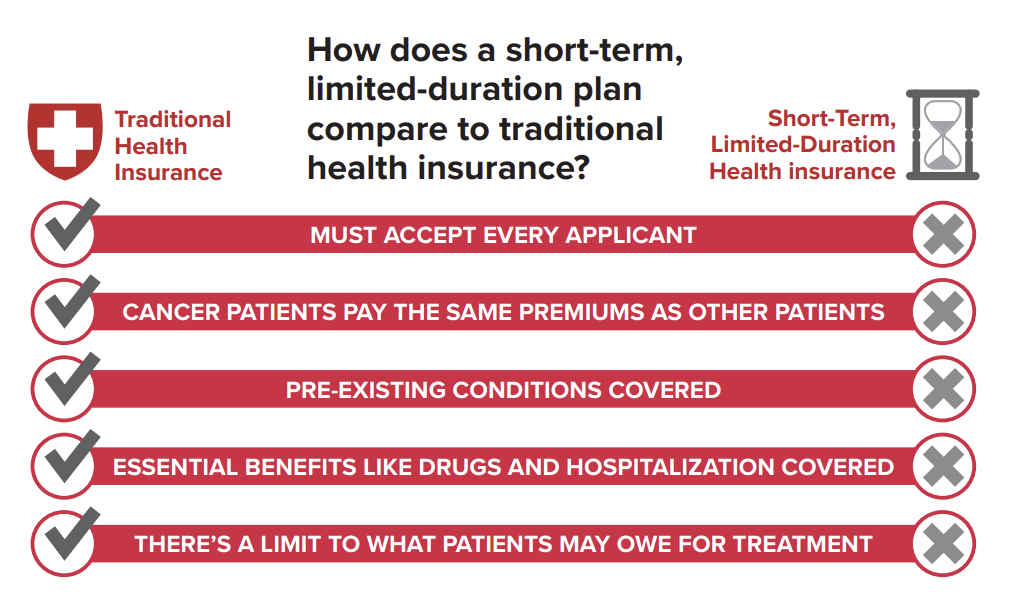
Proposed rules would protect consumers from junk insurance plans, surprise bills and medical debt
Junk insurance plans that don’t meet the standards of the Affordable Care Act are one of the biggest holes in…

-
How to cover the case that could kill patients’ access to no-cost preventive services
A key provision of the Affordable Care Act is in jeopardy in the case of Braidwood Management Inc. v. Becerra…