So far this year, hardly a week goes by without an article or report on egregious actions by nonprofit hospitals. While the actions aren’t new, several factors have combined in 2023 to raise the level of scrutiny.
Stories about what the nonprofits have been up to are relevant to audiences across the nation as almost 3,000 of the nation’s 5,157 hospitals are nonprofits, meaning the IRS views them as charities if they meet federal and state guidelines. Under these guidelines, nonprofit hospitals are exempt from paying federal and state income tax, sales tax, and property tax, and get other tax-related benefits such as the ability to issue tax-free bonds, as researchers in Health Affairs reported in 2021. Those guidelines mean that nonprofit hospitals are held to higher standards than the 2,157 for-profit and public hospitals.
Nonprofit hospitals are an important story to cover for these four reasons:
- While nonprofits do not need to pay federal or state taxes, they still generate income, as Michelle Crouch reported in April for North Carolina Health News and the Charlotte Ledger. Property that Atrium Health owns in Charlotte, N.C., houses a PDQ fried chicken restaurant. “You’ll pay taxes when you buy the chicken tenders, but Atrium doesn’t pay taxes on the land the restaurant sits on,” she wrote.
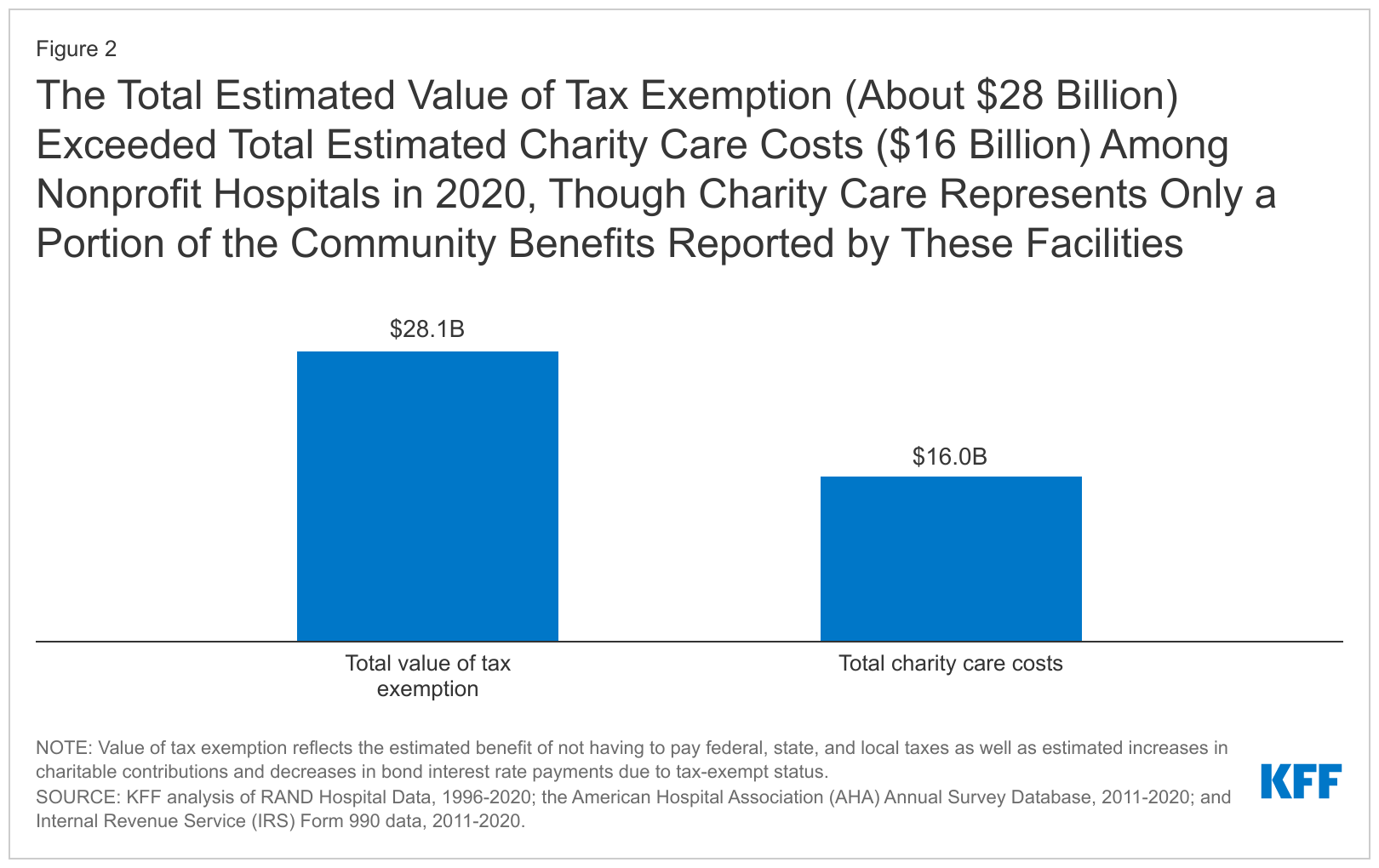
- In exchange for not paying income or property taxes, hospitals say they provide millions in discounted medical care to the underserved. But when health care journalists review the finances and charity-care spending of these facilities, nonprofit hospitals often fail to meet these requirements. In a report in March, KFF researchers estimated the value of tax exemptions for nonprofit hospitals was about $28 billion, exceeding the estimated charity care costs of about $16 billion among those hospitals in 2020.
- A June report from Human Rights Watch shows how lax federal oversight allows private tax-exempt hospitals to spend far less on health care for the poor than the public subsidies they get. Such tax exemptions are designed to increase access to care for uninsured and underinsured patients, but those subsidies are poorly regulated. This allows for abusive medical billing and debt-collection practices, according to the report.
- For KFF Health News, Andy Miller and Markian Hawryluk reported in July that more than a dozen states have considered or passed laws to define charity care more specifically, to improve transparency about the benefits hospitals provide, or to set minimum financial thresholds for charitable help in the communities the hospitals serve.
Rising rates of consumer medical debt has increased interest from lawmakers, the public and journalists, Miller and Hawryluk reported. More than 100 million Americans have medical bills they can’t pay, many of which were from nonprofit hospitals, according to a June 2022 KFF Health News article.
Essential tools for reporting on nonprofits
Reporting on nonprofit hospitals requires painstaking diligence to ensure that all facts are correct because hospital administrators won’t hesitate to challenge inaccuracies. Therefore, health care journalists need resources to cover this issue well, including the following:
- The names of nonprofit hospitals, their annual revenue and amount spent on charity care (also called health equity).
- An understanding of hospital finances during and after the pandemic.
- Good examples of how other journalists have covered these issues.
One of the best sources for the names of nonprofit hospitals is the Lown Hospital Index. Updated in July 2023, Lown’s list of America’s Most Socially Responsible Hospitals showed that among 3,637 hospitals, only 54 had the highest grades on equity, value and outcomes. This list is useful for journalists seeking hospitals with the highest grades, how pay for chief executives correlates with Lown’s social responsibility rankings, and more.
Keep in mind that hospitals need to codify and post their rules for offering discounted or free care in financial assistance policies, but most states do not specify how hospitals should implement those policies, according to a Lown Institute report.
Since December, Lown has published two reports on financial assistance: “Fair Share Spending,” showing how much 1,723 nonprofit hospitals give back to their communities; and “How some hospitals put up barriers to financial assistance.”
Another source is the annual U.S. News and World Report ranking showing the best hospitals on multiple measures, including a health equity score added last year. The publication evaluated health equity in four areas:
- Racial disparities in unplanned readmissions;
- Charity care provided to uninsured patients;
- Community residents who received care;
- Preventive care for Black residents in the community.
See, for example, how investigative reporter Molly Castle Work uncovered lawsuits filed by the Mayo Clinic against patients after Mayo was named the top hospital in the nation last year but scored poorly on health equity.
Understanding hospital finances
Journalists also need to evaluate hospitals’ finances both before and after the pandemic, according to AHCJ member Karl Stark who spoke at Health Journalism 2023 in March. View Stark’s presentation from the conference below.
(Editor’s note: The AHCJ resource hospitalfinances.org is being rebuilt and should be back online this fall.)
A former editor at The Philadelphia Inquirer, Stark is the director of content strategy for the Leonard Davis Institute at the University of Pennsylvania.
“When reporting on nonprofit hospital finances, first check any lawsuits the hospital system has filed against patients for unpaid bills,” said Stark in a telephone interview. Finding such lawsuits against patients can be difficult because hospitals often file these claims under the names of third parties, he added.
“You can’t just look up the name of the hospital,” Stark said. “Instead, interview lawyers doing bankruptcy work or those who represent people with medical bills and who know how hospitals are suing people.”
Other resources for covering nonprofit hospitals
- In 2020, two journalists from Kaiser Health News (now KFF Health News), former senior correspondent Jay Hancock and former data editor Elizabeth Lucas, were Pulitzer Prize finalists for reporting on the predatory billing practices of the University of Virginia Health system, a state-owned nonprofit. See this article, “UVA Health filed 36,000 lawsuits against patients,” and “Pulitzer finalists explain how to use court documents to cover hospitals’ predatory billing practices.”
- Last year, Anna Wilde Mathews, Tom McGinty and Melanie Evans reported on this issue for The Wall Street Journal, Big Hospitals Provide Skimpy Charity Care — Despite Billions in Tax Breaks.
- Among the best examples of journalists covering nonprofit hospitals was a series last year in The New York Times titled Profits Over Patients.
- Nonprofit hospitals often say they struggle financially, which may be true since federal COVID-19 funding has ended and stock market returns were poor. On this issue, see these two articles from Health Affairs: “What’s Behind Losses At Large Nonprofit Health Systems?” and “Nonprofit Hospitals: Profits And Cash Reserves Grow, Charity Care Does Not”.




