Tag
underinsured
-
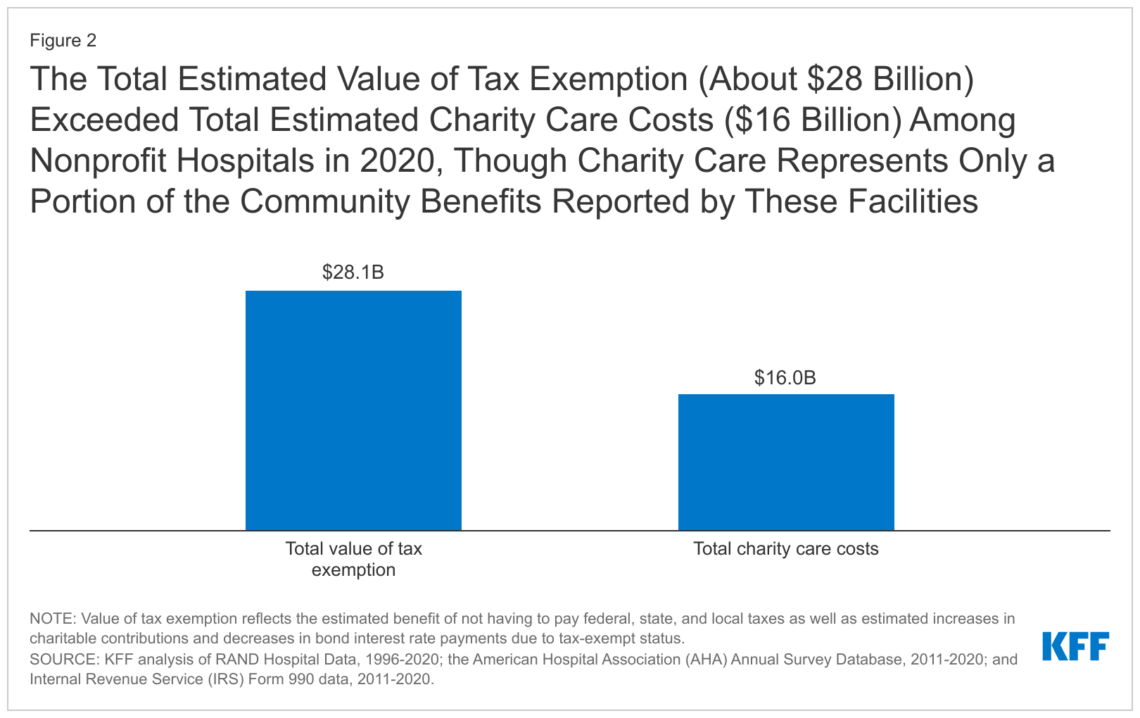
Tip sheet: Nonprofit hospitals are gaming the system at patients’ expense
So far this year, hardly a week goes by without an article or report on egregious actions by nonprofit hospitals.…

-
Being ‘underinsured’ another measure of health coverage
This year the rate of those who are uninsured has risen steadily, as the Gallup Sharecare Well Being Index shows.…

-
MMWR: Mass. reform narrowed insurance gap
Studying data from the Massachusetts Behavioral Risk Factor Surveillance System has led researchers to conclude that health care legislation in…

-
Underinsured face higher bills, bankruptcy
In Time, Karen Tumulty used the story of her brother’s kidney problems and resulting medical bills to look into the…

-
Three health-care issues Obama, Congress will face
The NewsHour with Jim Lehrer recently ran three stories about some of the health care challenges that President-elect Obama and…