Tag
surgery
-
Impossible odds persist for many on organ transplant waitlist
Getting an organ transplant is a game of chance where your odds depend on the color of your skin, the…

-
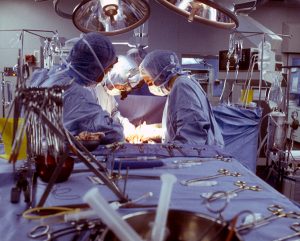
Despite checklists, cataloging strategies and other efforts, ‘forgotten surgical items’ remain a problem
About this time every year, the story of Dan Jennings, a man I got to know fairly well, always seems…

-
New data resource on NSQIP database can inform coverage of relevant medical studies
More than 1,500 peer-reviewed studies have relied on a surgical database known as the National Surgical Quality Improvement Program (NSQIP),…

-
VA surgery database explanation available for medical research reporting
Surgery research can become complex very quickly: Not only are there the underlying conditions and demographics of each patient to…

-
•
Child’s death highlights effort to reduce risks of dental surgery
Three-year old Daleyza Hernandez-Avila died on June 12 after being placed under general anesthesia at a Stockton, Calif., dental surgery…

-
Keep in mind unintended consequences of price transparency
It’s always a good idea for reporters to think about unintended consequences, especially when we’re talking about the latest, trendiest…

-
Report shows how reference pricing brings down costs
One issued we pursued during the AHCJ webcast last month (The cost of health care: Is transparency possible?) is whether…

-
•
Doctor: News coverage of face transplants has helped donors’ families to consent
This is a guest post from AHCJ member Chelsea Conaboy that first appeared in “White Coat Notes” at Boston.com. By…

-
•
NYT reporters tease hip replacement numbers from difficult data
Writing for The New York Times, Barry Meier and Janet Roberts analyzed a particularly tricky batch of federal reports detailing…

-
•
Laser spine clinics use Internet search ads to push unproven, costly treatment
Bloomberg’s David Armstrong has put together an investigation of a simple, effective and dubious new business formula, one which begins…