Tag
social determinants of health
-
Digital determinants of health important with growing technology usage
Digital determinants of health could include factors like ease of use, interactivity, digital literacy, broadband access and more.
-
These tools add important social context to public health stories
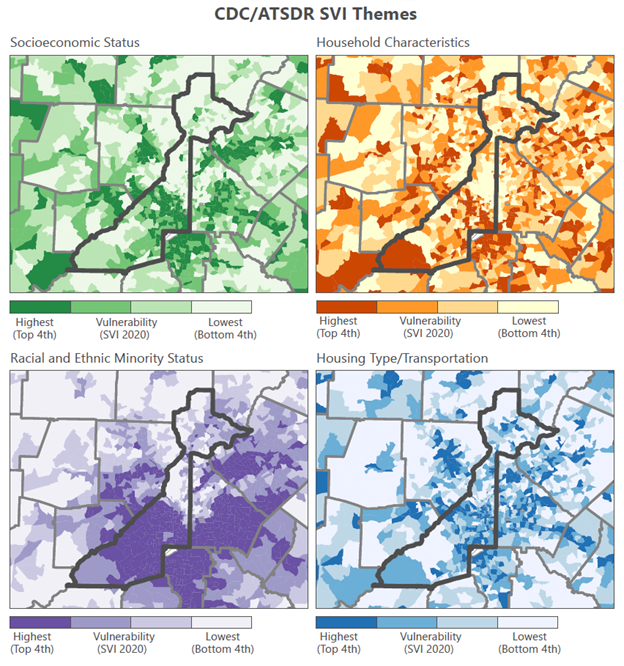
Federal, state and local officials use risk assessment tools called “social vulnerability indices” to identify places that may be hit…
-
Reporting on COVID-19 and obesity
The childhood obesity epidemic was one of the biggest public health stories before the pandemic and remains an important topic…
-
Groups aim to reinvent neighborhoods with eye on health
Amid growing awareness about “ZIP code” health disparities, some struggling areas are trying new ways to reinvent their communities and…
-
ZIP code vs. genetic code: How to cover health inequality #ahcj15
Poverty is a poignant reality – and an overwhelming one. If you’re a reporter, you might struggle to find the…
-
What’s really driving health inequalities
The U.S. and other wealthy nations have practically eliminated all of the infectious diseases that seemed to account for the…
-
Reporter crafts story about connections between poverty, illness
It didn’t sit right with Olga Khazan, an associate editor at The Atlantic, seeing so many people focus on individual…