Tag
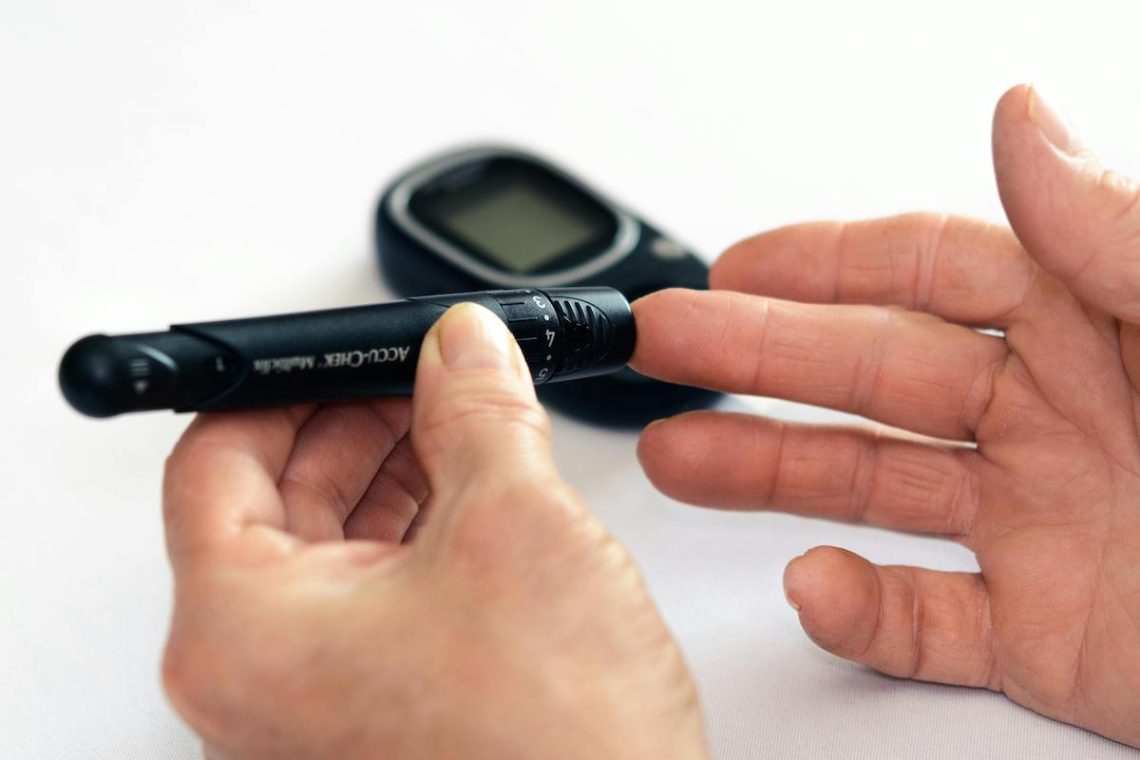
medical devices
-
Medical device manufacturers often delay reporting adverse safety events, study says
A recent study found late reports of deaths, injuries and device malfunctions from medical device makers. Who will review these…

-
FDA to launch ‘active’ monitoring system to improve medical device safety
The new system aims to detect potential safety issues with medical devices nearly in real time by monitoring data like…

-
Summit of tech giants takes on the cloud and improving patient data interoperability
At a developer conference hosted at the White House last week, six of the biggest tech companies issued a joint…

-
What to ask hospitals about medical device hacking preparedness
It’s only a matter of time before a patient is harmed through medical device hacking, and journalists have many resources…

-
Study suggests FDA medical device approvals ripe for investigative dives
Medical devices — and the unrecognized or undisclosed risks some of them have — have been in the news quite…

-
How will the election affect the business of health care?
The Washington Post has taken a post-election look at 15 major industries in a story aptly titled, “Mr. Business Goes…

-
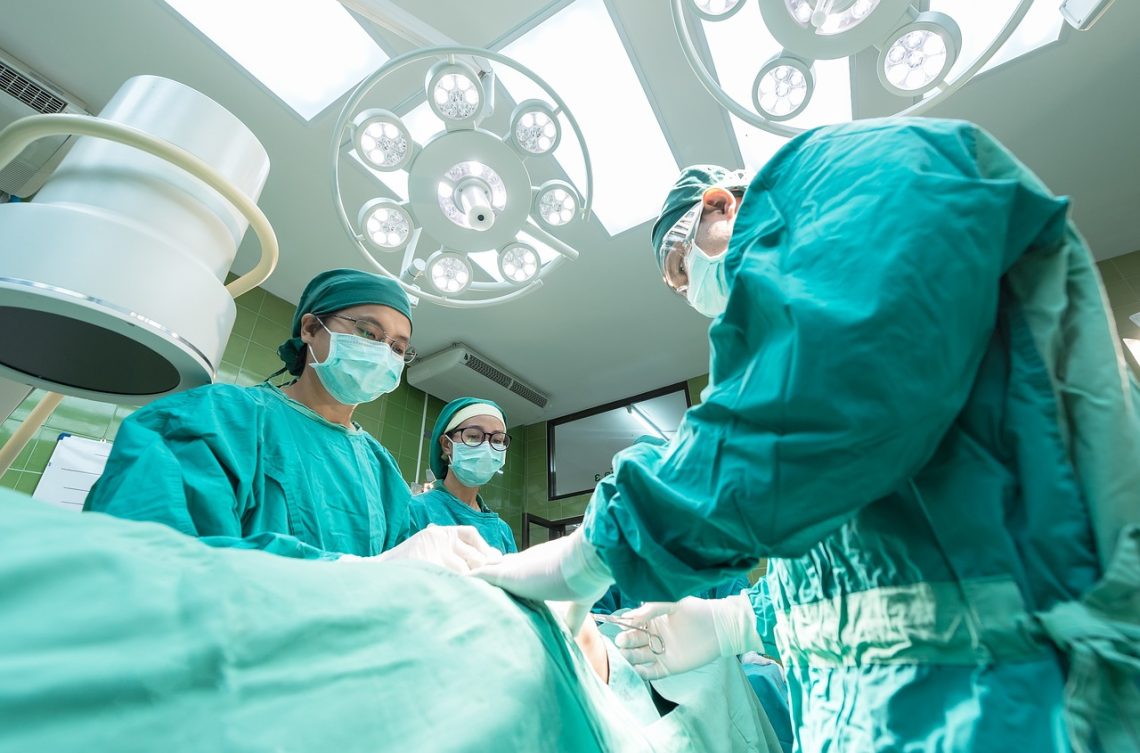
Evidence-based reporting leads to award-winning exploration of robotic surgery
Robotic surgery has exploded in popularity in recent years, but is that because it actually improves patient outcomes over traditional…

-
Controversy over breast implants spreads across Europe
British clinics delivering cosmetic surgery were thrown into crisis by the decision last month of the French government to fund the removal…

-
•
New Wisc. rules lead to interesting disclosures
Thanks to new disclosure requirements from the University of Wisconsin’s doctor group, the Wisconsin State Journal‘s David Wahlberg was able…

-
•
Fauber finds ‘failed back surgery syndrome’ after off-label use of Medtronic’s Infuse
John Fauber follows up his previous investigations into the myriad problems and conflicts of interest surrounding Medtronic’s Infuse product with…