The coronavirus has certainly pushed the health care system into a crisis. Still, even before the pandemic began earlier this year, health insurance coverage in the states already was being eroded and health care costs were rising sharply along with the number of preventable deaths, according to a new report by the Commonwealth Fund.
In addition to those sad statistics, the fund’s researchers show in the 2020 Scorecard on State Health System Performance that racial and ethnic disparities were getting worse as well.
One significant implication of the report is that it highlights deficiencies in the health care system that have left the nation far less prepared than other wealthy nations to deal with the COVID-19 pandemic, the authors note. What’s more, the pandemic is likely to make these trends worse because unemployment will rise and the use of health care services will drop, they added.
As a useful resource for health care journalists, the report assesses all 50 states and the District of Columbia on 49 health care measures, including access to care, health care quality, the costs of care, patient outcomes, and income-based health care disparities. Also, it identifies a range of deficiencies in the health care system in each state that the coronavirus pandemic has exacerbated.
Using the 49 measures, the researchers ranked the states, reporting that Hawaii, Massachusetts, Minnesota, Iowa and Connecticut were in the top tier while West Virginia, Missouri, Nevada, Oklahoma, and Mississippi were at the bottom.
On the webpage where the full report resides, the authors added have linked to a zipped file with a two-page summary for each state, appendices to the report and the press release.
Since the report as released Sept. 11, journalists have written about how their state measures up.
For Georgia Health News, Andy Miller reported that the state had slipped from a rank of 42 last year to 46th place among the states in the latest ranking.
Corey Jones reported for the Tulsa World that Oklahoma’s health system was ranked next to last but is primed for improvement. “Voters narrowly approved State Question 802 on June 30 to enshrine Medicaid expansion in the Oklahoma Constitution,” he wrote. “Prior to the COVID-19 pandemic, an estimated 200,000 low-income Oklahomans were expected to be eligible for the health insurance program when it becomes effective July 1, 2021.”
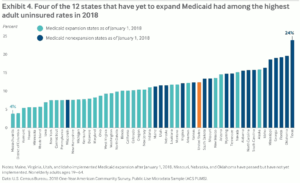
Jones then went a step further, pointing out how two neighboring states, Texas and Colorado, fared in the report. Texas, with an uninsured rate of 24 percent, was the only state with a higher uninsured rate than Oklahoma and has not expanded eligibility for Medicaid enrollment under the Affordable Care Act (ACA). In comparison, the uninsured rate in Colorado is 10 percent, and that Colorado did expand its Medicaid program in 2014.
The report’s authors also focused on Medicaid expansion, explaining that in 2018, the uninsured rates were among the highest in the nation in four of the states that had not expanded Medicaid eligibility: Florida, Georgia, Mississippi and Texas.
In two states that expanded Medicaid eligibility relatively late, Alaska and Louisiana have reported the largest state declines in uninsured rates since 2016, the authors wrote.
While the ACA helped to reduce the number of uninsured Americans since it went into effect in 2014, those gains have stalled and are being eroded in most states, the report shows.
“Between 2014 and 2016, every state saw at least a 2 percent annual reduction in uninsured rates,” the researchers wrote. “Since 2016, 23 states saw those gains flatten and 22 saw uninsured rates creep up.”
Worsening disparities
Not only did the ACA reduce the number of uninsured, but it also had a crucial role in reducing income inequality and racial and ethnic disparities, the report shows. But again, those improvements have stalled since 2016. “In 2018, the uninsured rate for Black and Latino adults in 17 states was at least five percentage points higher than it was for white adults,” the authors report.
The researchers found another disparity in life-expectancy data, writing that treatable conditions are causing Americans to die earlier than expected from treatable conditions such as suicide, alcohol use and drug overdoses. Arkansas, Kentucky, Mississippi, New Mexico and Oklahoma had the biggest increases in premature death rates from 2012 through 2017, they add.
Life expectancy has declined for all Americans since 2014, but Blacks are twice as likely as whites to die from treatable conditions. “Black Americans, who also have suffered disproportionately during the COVID-19 pandemic, were twice as likely as whites to die early from treatable conditions such as diabetes, heart disease, appendicitis, and certain cancers,” the authors wrote. While such disparities are common in every state, Arkansas, Mississippi and Oklahoma reported the highest rates of premature deaths among Black Americans, the report shows.
Journalists may be interested to note that this year, the report includes
additional data on price information for health services in the states, state-based public health spending and primary care spending among Medicare beneficiaries and those with employer coverage.
Authors of the report were Sara R. Collins, the fund’s vice president; David C. Radley, a senior scientist; and Jesse C. Baumgartner, a research associate.




