Tag
risk
-
Assessing infectious disease risks and impact of social media
During an infectious disease outbreak, how does a journalist provide accurate information about risks to the public as the event…

-
Australian physician-journalist offers pearls for health journalists
One of the best ways to become a better health journalist is to find out what the best in the…

-
Increased optimism about new Alzheimer’s drugs, tests
You may have recently heard about the multimillion-dollar donation that Bill Gates and Leonard Lauder made to support research into…

-
‘Short-term’ plans can now be renewed for years
In my most recent post, I recapped what Georgetown University’s Sabrina Corlette, who is also a former Senate health policy…

-
Research: Finesse, transparency key when reporting foodborne illness outbreaks
A mainstay of health reporting is covering outbreaks of foodborne illness, whether it’s salmonella in peanut butter (and its criminal…

-
Tip sheet series to focus on red flags to look for in medical studies
With thousands of medical studies published every day, it’s impossible to cover even 1 percent of them. When you can…

-
Context, context, context: How journalists can avoid confusing readers with the latest research findings
A recent editorial in the Journal of the American Medical Association explored the responsibility that journals have to public health…

-
Return to McAllen illustrates changes ACA has brought to health care system
In June 2009, Atul Gawande wrote an influential New Yorker article, about the community of McAllen, Texas, which has some…

-
•
Frailty affects quality of life, makes seniors more vulnerable
The term “frailty” seems to be practically synonymous with aging. And while it’s true that adults naturally have a gradual…

-
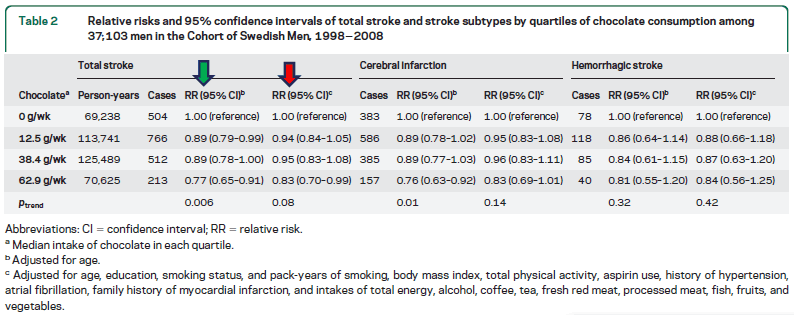
Don’t fudge the facts on chocolate studies
Studies that support a link between chocolate and good health are popular with readers. But the reality is that most…