Tag
income
-
NYT maps how high health gaps lower the odds
The impact of “income inequality” has been given a closer examination since the recession and is teeing up as a…

-
•
Complaints about dental benefits provider mounting
The rumblings in Tennessee started earlier this year, after a new company took over the contract to provide dental services…

-
A ‘birth lottery’ still determines who gets to live longest, healthiest life
“Since when in America do we have classes? Since when in America are people stuck in areas or defined places…

-
Drilling down into numbers uncovers Marketplace glitch
Ten days before the (expected) close of open enrollment, The Philadelphia Inquirer reported that the federal exchange’s window-shopping tool – the one…

-
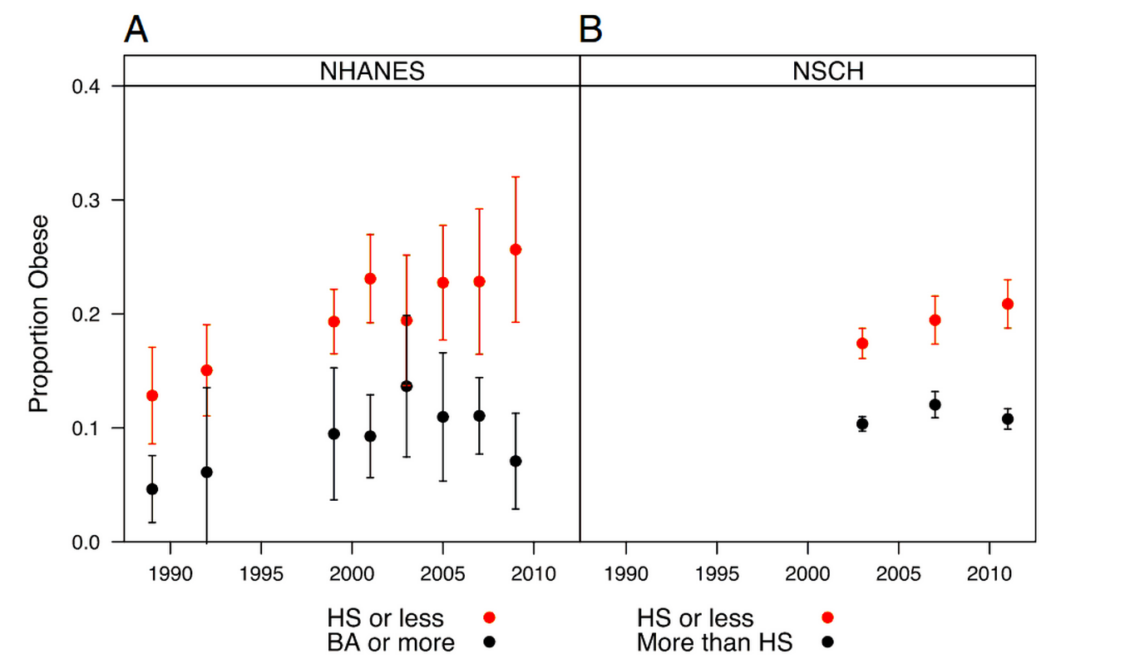
Uncovering the real drivers of obesity in young people
It’s great that the rapid rise in youth obesity since the 1980s has started to level off. But there’s an…