Tag
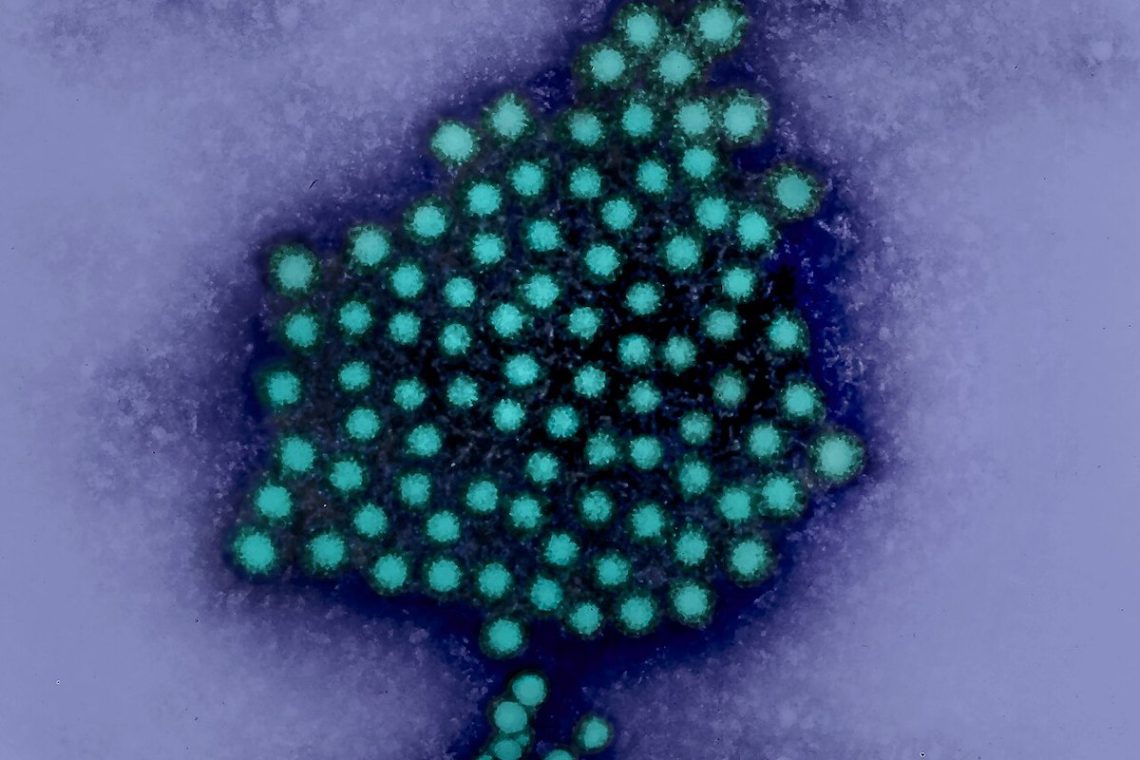
hepatitis
-
How to cover hepatitis in your community
Hepatitis is a significant public health burden that reporters need to cover, so here are ideas for local coverage and…

-
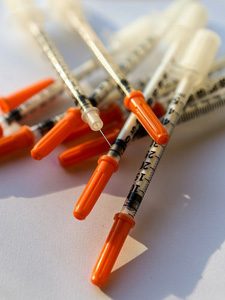
Infectious disease rates rising with opioid epidemic
As the opioid crisis has continued to plague the nation, a less-reported story for journalists to consider is the surging…

-
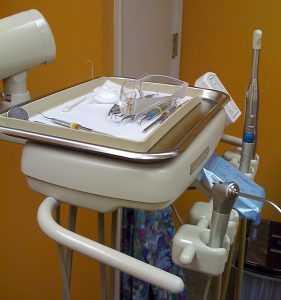
Investigations put focus on infection control in dental offices
Two high-profile safety breaches have highlighted the importance of close adherence to infection control protocols in dental clinics and offices.…

-
Connecting the dots between social determinants and infectious diseases
Socioeconomic factors such as poverty and living conditions play a role in shaping infection risk and disease outcomes. Many times…

-
Infectious disease outbreaks rise with opioid epidemic
Cases of infectious diseases such as hepatitis A, B and C, sexually transmitted diseases (STDs) and human immunodeficiency virus (HIV)…

-
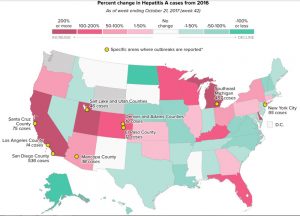
HuffPost reporter, drawn by data, paints larger picture of hepatitis outbreak
It was supposed to be a simple map. But what started as a small graphics project at HuffPost soon transformed…

-
Signs of housing shortages in other cities evoke West Coast crisis
The deadliest outbreak of hepatitis A in the country flaring in southern California stems from a confluence of factors, from…

-
In California, housing crunch exacts toll as hepatitis deaths grow
Along the southern California coastline, surging development has triggered a housing boom that has also come at a heavy price…

-
Eight-part series on hepatitis C finds unique moment in an epidemic
While working on a documentary about opioid addiction, Kristin Espeland Gourlay, the health care reporter for Rhode Island Public Radio, discovered…

-
Hepatitis cases highlight infection control for temporary dental clinics
It is likely that three patients and two volunteers contracted hepatitis B at a large free dental clinic held in…