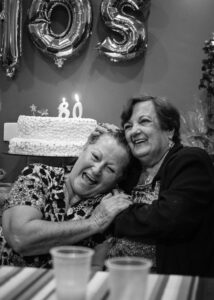Tag
depression
-
Clinicians: New federal guidance on anxiety screenings don’t do enough to curb youth and young adult suicide
The U.S. Preventive Services Task Force has received credit for bringing awareness to the possible links between anxiety and other…

-
Lack of Medicare Advantage mental health providers means seniors’ needs often go unmet
New study finds people on Medicare Advantage have narrower networks for psychiatric care and more difficulty finding and accessing mental…

-
Resilience factors in older women could hold key to better quality of life
Study finds older women with more education and less stress have more resilience in older age.

-
38% of those screened for depression reported suicidal thoughts amid COVID-19
The first of four briefs Mental Health America will release in 2021 has concluded that 38% of 725,949 people who…

-
New core topic leader explores importance of mental and behavioral health coverage
Coming up in my particular neighborhood in Little Rock, Ark., one of my dearest childhood friends was a boy we…

-
Panelists discuss challenges of reporting on mental health and older adults
Covering mental health issues among older adults first means understanding the differences between issues of social isolation, loneliness, depression, and…

-
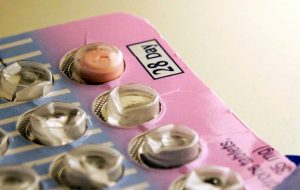
Confounding by indication case study 2: Hormonal contraception and risk of depression
I wrote in a previous blog about the importance of understanding confounding by indication and being sure to ask researchers…

-
Tip sheet highlights program addressing older adults’ mental health
Mental and physical health often go hand in hand, but for many older adults, mental health conditions can be missed…

-
Programs team up to help low-income seniors
Habitat for Humanity and Johns Hopkins have teamed up to implement the CAPABLE program, in six new areas across the…