Tag
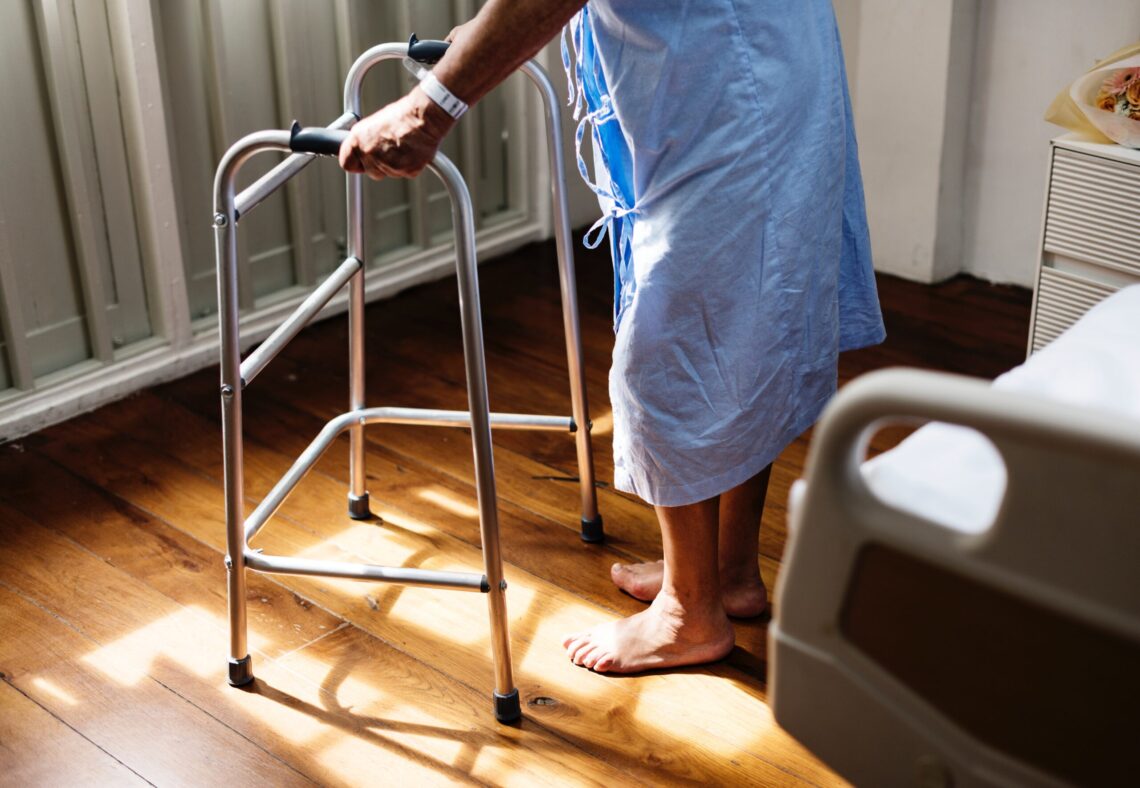
care coordination
-
Care coordination: why it matters
It’s one thing to report on a story from the outside. It’s quite another to see it from an insider’s…

-
Experts: Care coordination, medical homes key to tackling global aging issues
An aging population isn’t just a challenge for providers and policymakers in the U.S. – it’s an issue most nations…

-
Clearing up confusion about those enrolled in both Medicare, Medicaid
Dual eligibles are low-income elderly or disabled people enrolled in both Medicare and Medicaid. The distinctions are sometimes bewildering. It’s easy…

-
•
Survey: Older patients like, want medical homes
Older patients like the kind of team care delivered in medical homes and most of those who get this care…