For the first time, the government can begin negotiating drug prices directly with pharmaceutical companies under the Inflation Reduction Act of 2022. The first step in those negotiations begins Sept. 1.
The U.S. has tried and failed to rein in rising drug prices since at least 1993 when President Clinton introduced reform under the Health Security Act, as the late Robert Pear wrote for The New York Times. In that unsuccessful attempt, Clinton proposed allowing Medicare to use its negotiating power to win discounts from pharmaceutical companies.
“Until now, the United States stood alone among high-income countries with no government control (outside of Medicaid and the Veterans Health Administration) over drug prices,” KFF’s Larry Levitt explained in an op-ed last year. “That’s why prices in this country are roughly triple what other nations pay for the same brand name drugs.”
Health care journalists have a vital role in explaining how the Inflation Reduction Act works. While the Act is historic and broadly popular, its drug-pricing requirements are little known, as Rachel Roubein wrote for The Washington Post on Aug. 16, the one-year anniversary of the bill’s signing. It’s worth noting that since President Biden and the Democrats passed the Act without any GOP votes, some Republicans have taken credit for the law.
The Act’s broad provisions
In addition to allowing the federal government to negotiate drug prices, the Act is projected to save $98.5 billion over the next 10 years, according to the Congressional Budget Office.
Those savings will come from many provisions designed to keep drug costs low for older and disabled people enrolled in Medicare. This year alone, the law:
- Requires drug companies to pay rebates if prices for seniors’ medications rise faster than inflation.
- Limits monthly cost sharing for insulin to $35 for Medicare members.
- Eliminates cost sharing for adult vaccines under Part D.
- Improves access to adult vaccines in Medicaid and CHIP.
Next year, the law caps out-of-pocket spending under Part D and increases eligibility under Part D’s Low-Income Subsidy Program.
Drug company opposition
While these changes and the savings are important, the biggest news stories will come from the fight over drug price negotiations starting next month, as Sheryl Gay Stolberg and Rebecca Robbins reported for The New York Times. Pharmaceutical companies have argued that the law is unconstitutional, will harm drug-discovery efforts and do little to cut costs, as this April 2023 report from USC’s Leonard D. Schaeffer Center for Health Policy & Economics noted.
Despite this opposition, the U.S. Centers for Medicare and Medicaid Services will announce the names of the first 10 Part D drugs (those sold in retail pharmacies) to be subject to price negotiations by Sept. 1. These medications are likely to be for patients with such common conditions as diabetes, cancer, respiratory ailments and cardiovascular disease, according to a recent study.
Report shows rising drug prices
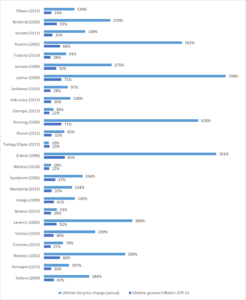
A timely new report from AARP’s Public Policy Institute shows that list prices for 25 top Medicare Part D drugs have increased by an average of 226% — more than three times their initial cost — since each entered the market. These increases are far higher than the rate of inflation over the past several decades.
Lifetime list price changes increased dramatically the longer a product was on the market, and nearly 60% of current list prices for these drugs came from price hikes after they were launched, the report showed. Among the highest cost drugs available for less than 12 years, the average increase was 58%, and the average lifetime increase for those on the market for at least 20 years was 592%. Two medications — Lantus (insulin) for diabetes and Enbrel (etanercept) for rheumatoid arthritis — increased by a whopping 739% and 701%, respectively, since their launch.
Why this matters
The study provides a backdrop to why the Inflation Reduction Act’s price negotiations are not only timely but overdue, according to Leigh Purvis, M.P.A., director of health care costs and access for the AARP Public Policy Institute. Price increases build on each other and add up over time, she said during an Aug. 10 media briefing.
“There is no justification for drug companies to engage in these types of price increases every year they’re on the market,” Purvis said.
Using data from CMS, the report showed that the Part D annual cost of the cancer drug Revlimid (lenalidomide) increased from almost $88,000 in 2017 to nearly $130,000 in 2021, a $40,000 jump. The AARP analysis is based on the 25 brand-name drugs with the highest total Medicare Part D spending in 2021, according to CMS.
Even a small increase adds a lot to a drug’s price because new drugs cost an average of $200,000 annually, Purvis said.
“Increasing drug prices will lead more older Americans to stop taking their medicines, which will lead to higher health care costs and poorer health outcomes in the future,” she added.
Tough choices: Food or drugs
Research shows those who struggle to pay for basic needs like food, housing and utilities may be unable to afford their prescription medications.
“Spending less on basic needs to pay for medication is a particularly concerning cost-coping strategy and may be associated with worse health outcomes,” researchers noted in a 2021 study.
Seniors on Medicare prescription drug plans take an average of four to five such medications each month, and many of those drugs require patients to pay a percentage of retail price. Most Medicare members with a standard drug benefit plan have an out-of-pocket spending cap of $7,400 in 2023, according to Medicare.gov. Those who lack prescription drug insurance must absorb these price increases on their own.
In a report last year, the HHS Assistant Secretary for Planning and Evaluation showed:
- An estimated 3.5 million adults 65 and older and 1.8 million Medicare beneficiaries under 65 had difficulty paying for their medications in 2019.
- Black and Latino adults over age 65 reported difficulty paying for prescription medications at rates roughly 1.5 to two times higher than white adults.
- Medicare beneficiaries under age 65, who generally qualify for Medicare with a disability or have end-stage renal disease, had much higher rates of affordability problems with prescriptions than adults over 65 did.
- Women, people with lower incomes and beneficiaries diagnosed with chronic conditions such as diabetes had higher rates of problems affording prescriptions than those in other groups.
Resources
- FAQs about the Inflation Reduction Act’s Medicare Drug Price Negotiation Program, a report from on Aug. 8, 2023.
- Older Americans Face More Cost-Related Access Barriers than People in Other High-Income Countries, report in 2021 from The Commonwealth Fund.
- Consumer Access to Affordable Medicines Is a Public Health Imperative, report in 2017 from the National Academies of Sciences, Engineering and Medicine.
- Medicare Part D Spending by Drug, drug price dashboard from CMS.