 Chronic pain is fairly common among older adults. Nearly half of community dwelling and up to 75 percent of institutionalized adults over 65 report some type of persistent pain. Coping with pain frequently involves a combination of prescription and over-the-counter medications, from NSAIDs to opioids. However, that approach can create a host of issues, including drug-drug interactions, balance and sleep problems, or addiction. Is there another way?
Chronic pain is fairly common among older adults. Nearly half of community dwelling and up to 75 percent of institutionalized adults over 65 report some type of persistent pain. Coping with pain frequently involves a combination of prescription and over-the-counter medications, from NSAIDs to opioids. However, that approach can create a host of issues, including drug-drug interactions, balance and sleep problems, or addiction. Is there another way?
As this story in the St. Louis Post-Dispatch aptly stated, pain management in older adults has to extend beyond painkillers. That’s where integrative medicine comes in.
It combines complementary, alternative and Western medical treatment in a holistic approach to managing older adults with chronic pain and other long-term conditions, according to Wayne Jonas, M.D., former director of the National Institutes of Health Center for Alternative Medicine. He said that while the “pills and procedures” approach is great for keeping people with acute health conditions alive, “we’re not so good at managing the chronic part, which is the largest part of what people suffer as they get older.”
Jonas, a practicing family physician and author of “How Healing Works,” thinks our health system needs to widen the lens on determinants of health. He wants clinicians to go beyond the immediate problem to incorporate lifestyle and health behaviors like nutrition, activity, sleep, and stress management, in tandem with strategic use of evidence-based alternative approaches like acupuncture, behavioral therapy and yoga. “We realize now it’s actually what gets at the best way of managing chronic illness,” he said in a phone interview.
Jonas will speak at Health Journalism 2018 on a panel about the newest efforts in integrative health on Saturday, April 14.
An estimated 25 percent of older adults aged 65 to 69 take five prescriptions daily for chronic conditions, and after age 70, nearly twice that many (46 percent) do so, according to this story in the Washington Post. Getting older adults off multiple medications is important, and a huge concern for those who care for them, as Paula Span reported in the New York Times. And while opioid abuse among older adults is not as prevalent as among younger populations, it’s still a serious problem as this NPR story explained.
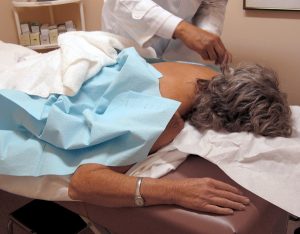
The body is complicated, and involves much more than biochemistry. Treating the whole person involves not only the physical components, but interaction with the environment and society. People need to have relationships and be part of a community, Jonas explained. “It’s the mind-body-spirit aspects that interact with each other to make up what’s valuable in life….” That’s especially true for older adults who often suffer from multiple chronic conditions at a time when they may also start becoming more socially isolated.
Older adults who suffer from chronic pain can incur substantial disability, including reduced mobility, activity avoidance, falls, depression, anxiety, and sleep disorders. This, in turn, may lead to social isolation. Pain management is further complicated by age-related physiologic changes, which lead to altered drug absorption and decreased renal excretion, as well as sensory and cognitive impairments, according to the NIH.
However, there’s growing evidence that non-pharmacological approaches to pain work.
“Some, like yoga, acupuncture, massage therapy, have been shown to be effective in good randomized control trials and they’re being recommended now. We need to figure out how to do that and patients need to ask about them,” Jonas said.
Integrative approaches to pain actually focus on creating health, not just curing the immediate, acute problem. This can mitigate and actually prevent a lot of chronic problems. Jonas explained. And evidence linking lifestyle interventions and pain management, such as movement, exercise, diet, sleep, stress and building resilience, is mounting. “These things have a huge impact, in fact they have a bigger impact than many of the drugs we use to manage many of the chronic diseases among older adults.”
Educators are taking notice too. The University of California, Irvine, recently revamped its entire medical education system, including its schools of nursing, medicine, pharmacy, and public health to create a new center for integrative medicine. Up the coast, Stanford University is using cognitive and behavioral therapy (CBT) techniques to help patients manage pain. It’s based on the idea that a person’s beliefs, attitudes and behaviors play a key role in how they experience pain. The University of Vermont’s College of Nursing is also developing an Institute for Health and Healing which adopts an integrative approach. Hospitals are also stepping up efforts to offer alternative medicine approaches to pain management, to the communities they serve, as the Beaumont, Texas Press & Guide reports.
According to Jonas, who has been practicing medicine for more than 40 years, “We have to get better at delivering whole person empathetic care as a culture, and doing it in a way that alters the physiology and actually produces hard outcomes.”
Journalists:
- Are hospitals or universities in your communities offering complementary or integrative health programs?
- Are more doctors and nurses adopting a “whole person” approach to care rather than just treating the acute problem(s)? What training or programs are available to them for complementary and alternative medicine?
- Talk to some local pharmacists, pain specialists, yoga practitioners, and acupuncturists. Are they seeing a lot of polypharmacy among older clients? Are alternative approaches helping to manage pain or other chronic conditions well enough for them to reduce or eliminate medications?
- This tip sheet offers information about chronic pain and aging.
The panel on integrative care is at 9 a.m. on Saturday, April 14. Follow along on Twitter with #AHCJintegrative.




