Tag
racism
-
Racial disparities in health linger, some rooted in fake science
During an HJ25 panel on racism in health care, panelists discussed how the residual effects of bad science and physician…

-
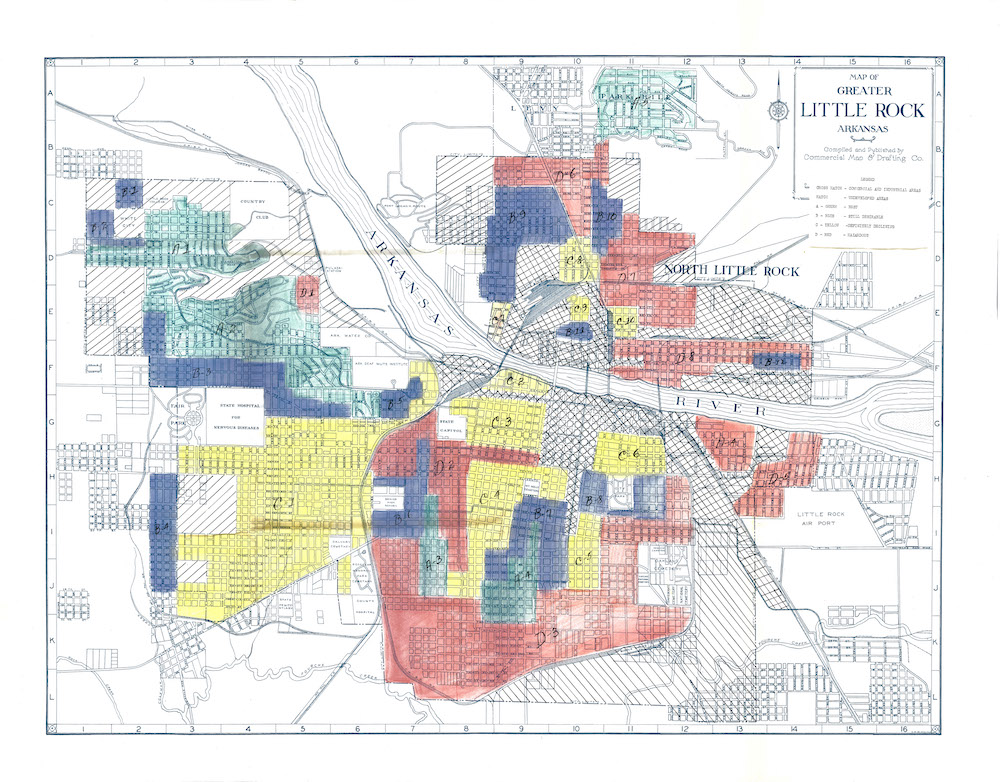
Redlining’s lingering public health legacy
Recent studies show that people from formerly redlined neighborhoods face multiple health disparities including a lower life expectancy.

-
Residents in certain ZIP codes are more likely to be fatally shot by police
A person’s ZIP code could determine their risk of being shot and killed by police, according to a recent study.

-
The complicated role race and ethnicity play in research
Using race and ethnicity categories in research contributes to health inequities — but omitting them can also be problematic, a…

-
How one reporter covered the removal of race from common algorithms
Learn how independent journalist Cassie Willyard wrote about efforts to update old algorithms and re-evaluate biased devices.

-
Biased devices: Reporting on racial bias in health algorithms and products
In this webinar, learn how these algorithms and devices work, how bias creeps in, the toll it takes, and efforts…

-
New book sheds light on legacy of physician, racism in medicine
During her book talk at HJ24, Dr. Uché A Blackstock reflected on her mother’s career in medicine as a first-generation…

-
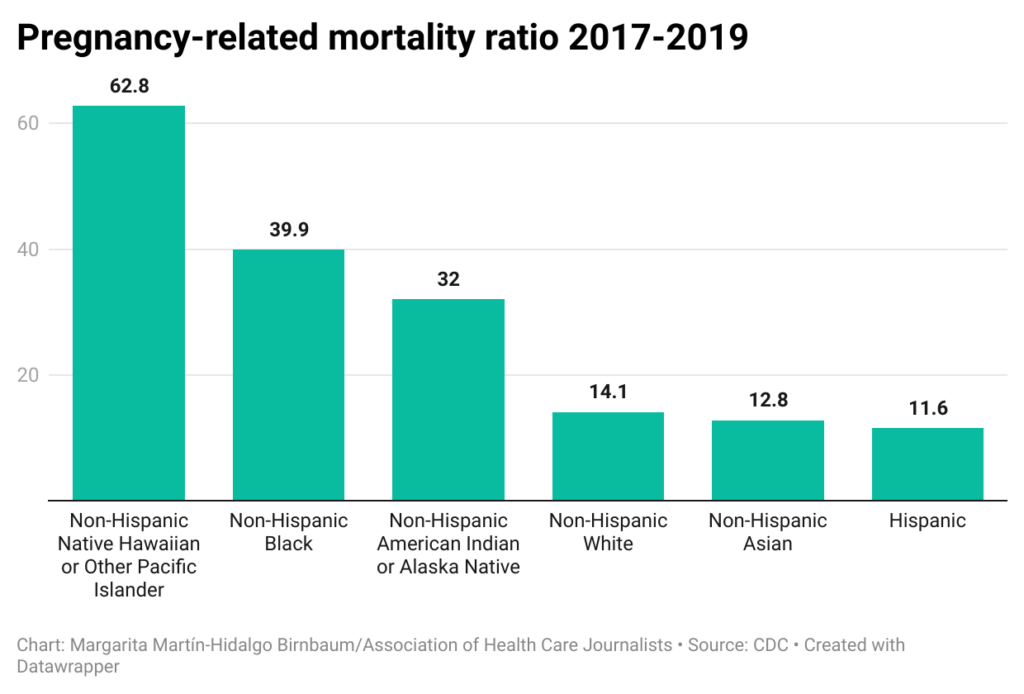
Finding fresh approaches to reporting on the maternal mortality crisis
A recent analysis of state maternal mortality data offers journalists topic ideas they can expand on in articles about a…

-
Before Tuskegee: An investigative project just waiting to happen
Many Americans know the story of the Tuskegee Syphilis Study, but most are likely unaware of the Julius Rosenwald Fund…

-
5 reports look at causes of health disparities in the U.S.
Stories about health disparities — even ones about CDC statistics — need context about the social causes that contribute to…