Tag
pandemic
-
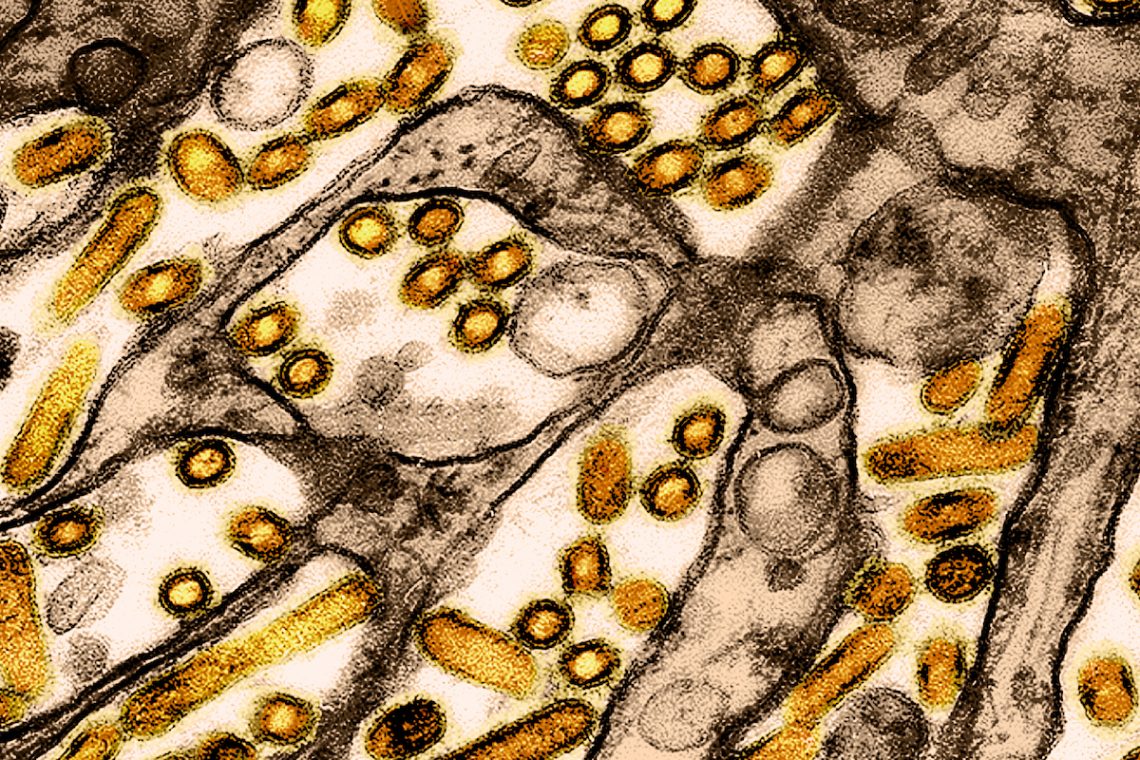
Covering bird flu from an ecological angle
Bird flu coverage shouldn’t be limited to what’s happening in birds, cows and humans — make sure to look at…

-
Covering the ongoing bird flu story as it unfolds
Check out these tips for reporting on the ongoing bird flu outbreak, including how to seek out undercovered stories and…

-
Brazen pandemic-era discrimination spurred new protections for patients with disabilities
Pervasive bias in the health system against patients with disabilities became glaringly apparent during the COVID-19 pandemic.

-
Loneliness and health inequity are post-COVID-19 stories to cover, reporter says
A Q&A with freelance writer Fran Kritz on covering the pandemic for NPR and story ideas after the global health…

-
More resources on variants for your COVID-19 reporting toolbox
Back in January, Bara Vaida, the AHCJ core topic leader for infectious disease, wrote a helpful post on resources for…

-
Fixing the public health system for the next pandemic
The American Rescue Plan (ARP), passed by Congress last month, will be sending about $100 billion into the U.S. public…

-
Mental health services benefitting from telehealth expansion during pandemic
Amid the mental and behavioral challenges fueled by COVID-19, expanded telehealth capabilities have contributed to a surge in mental health…

-
How one journalist pivoted her writing during the pandemic
At the beginning of the pandemic, Stephani Sutherland, a freelance writer focused on chronic pain issues, was — like many…

-
Resources for journalists covering COVID-19 “long-haulers”
COVID-19 has been around for just a year, so research about the long-term impact of the disease is sparse, but…