Tag
oklahoma
-
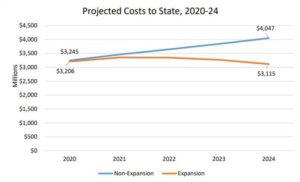
What Missouri, Oklahoma teach us about state efforts to expand Medicaid eligibility
Missouri voters in August approved a ballot measure that would expand Medicaid eligibility to include healthy adults, beginning July 1,…

-
Reporter explores how state’s economic health affects its oral health
The Oklahoma newspapers in the Community Newspaper Holding Inc. (CNHI) chain offered readers a series that examines the everyday challenges…

-
•
Newspaper’s economic health series explores role of oral health
The oral health of a state or community can serve as an interesting lens for examining economic health. That is…

-
Story highlights parents affected by state decision on Medicaid expansion
Ron Jackson of Oklahoma Watch wrote one of the best stories I’ve seen laying out the policy dimensions and the…

-
•
Tulsa World investigates billing, compensation at ambulance utility
The Tulsa World‘s Ziva Branstetter has, for months now, been doggedly investigating the billing practices of the Emergency Medical Services…

-
•
With state funds gone, Okla. dental programs still serve needy
Writing for the local NPR StateImpact outlet, Logan Layden looks at how dental programs for the needy are coping in…

-
Behind Oklahoma’s nation-leading access-to-care problems
In February, the New England Journal of Medicine ranked Oklahoma as the worst when it came to access to medical…

-
•
Papers combine forces to investigate group homes
Reporters from The Oklahoman and the Tulsa World teamed up to report on Oklahoma’s residential care homes and “Intermediate Care…

-
Medical tourism expected to continue growth
The San Francisco Chronicle‘s Carolyn Lochhead writes that the draw of medical tourism lies with both transparency and affordability and…

-
Bundled payments may improve care, lower costs
Kaiser Health News’ Phil Galewitz looks at bundling hospital payments, a possible solution to the confusion and cost of separate…