Tag
nursing home
-
Aging advocates brace for uncertain future
Longtime D.C. policy insider Bob Blancato briefs aging advocates on what to expect in federal aging policy for 2026 and…

-
New study highlights lack of nursing home medical director presence
More than one-third of nursing homes had no on-site medical directors present during the first quarter of 2023, a new…

-
Tip sheet: A quick primer on long-term care
Here’s what to keep in mind when reporting on the potpourri of federal, state and local long-term care programs, services…

-
How we did it: Uncovering abuse in Arizona assisted living facilities
Reporters Caitlin McGlade and Sahana Jayaraman found a disturbing trend of neglect, abuse and homicide at Arizona assisted living facilities.

-
Green Houses: A communal approach to elder care
Green Houses are elder-centered, long-term care residences that are designed to look and feel like a typical residential home.

-
Biden’s bid for a nursing home vaccine mandate faces obstacles
EDITOR’S NOTE: This is the second in a series about the Biden Administration’s efforts to increase COVID-19 vaccination rates among…

-
Reporter takes readers inside a nursing home’s effort to fight COVID-19
At the start of the COVID-19 pandemic, nursing homes throughout California were preparing for a wave of cases. Older adults,…

-
Staffing levels, not just hotspots, can predict nursing home COVID deaths, study says
Since the first COVID-19 outbreak in a Seattle-area nursing home in February, at least 55,000 deaths, more than 42% of…

-
How can states keep nursing home residents safe during the pandemic?
When we first learned of widespread incidence and deaths from COVID-19 in a Seattle-area nursing home, many in the aging…

-
•
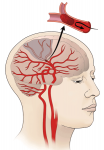
Men without caregivers at greater risk for nursing home placement following stroke
Male stroke survivors over age 65 may be three times as likely to end up in a nursing home within…