Tag
missouri
-
Inform your reporting on gun ownership with the ‘Missouri Firearms Survey’
While this survey only covers Missouri, it’s a useful snapshot to show how informed people are about firearms and the…

-
AHCJ’s 2023 conference to be held in St. Louis in March
Mark your calendar — we’re meeting in St. Louis! I’m pleased to announce that AHCJ’s annual conference will take place…

-
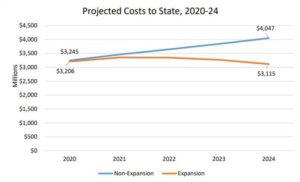
What Missouri, Oklahoma teach us about state efforts to expand Medicaid eligibility
Missouri voters in August approved a ballot measure that would expand Medicaid eligibility to include healthy adults, beginning July 1,…

-
•
Your money or your life? Missouri town had to choose
On KBIA public radio, Jacob Fenston tells the story of a Missouri town faced with a brutal, impossibly high-stakes catch-22.…

-
•
Joplin hospital staff took action during disaster
If you haven’t already, take 90 seconds to read Tulsa World reporter Michael Overall’s brief, powerful account of how emergency…

-
•
Skyrocketing drug price is chance to examine manufacturing, FDA approval process
St. Louis Post-Dispatch reporter (and Midwest Health Journalism Program Fellow) Jim Doyle has put together a series of stories on KV…

-
•
ER scribes handle EMRs, free up doctors
St. Louis Post-Dispatch reporter Michele Munz has found that some emergency rooms are easing the transition to electronic medical records…

-
New health-related state laws for 2011
Many thanks to Melissa Preddy for pointing out, in a post on the Reynolds Center’s businessjournalism.org, the National Conference of…

-
St. Louis reporters find felons practicing medicine
The St. Louis Post-Dispatch‘s Blythe Bernhard and Jeremy Kohler tell the story of an ophthalmologist to show how a convicted…

-
•
Rise, fall of two St. Louis pharma companies
Midwest Health Journalism Program fellow Jim Doyle, a reporter at the St. Louis Post-Dispatch, tells the story of Forest Pharmaceuticals…