Tag
fda
-
How STAT’s Lizzy Lawrence covers the quickly evolving FDA
Lawrence shares how she developed her beat covering the FDA and what she thinks local reporters need to pay attention…

-
What journalists should know about lab-developed tests
In March, a federal court invalidated FDA regulations on lab-developed tests. Your audience needs to know the implications of this…

-
Medical device manufacturers often delay reporting adverse safety events, study says
A recent study found late reports of deaths, injuries and device malfunctions from medical device makers. Who will review these…

-
Reporting duo investigates industry sway over the FDA
Reporters Jeanne Lenzer and Shannon Brownlee discuss their latest work, a three-part series on industry influence at the FDA.

-
Tips for covering the controversy surrounding pulse oximeters
The FDA just released new guidance on pulse oximeters after decades of studies showed how they don’t work well on…

-
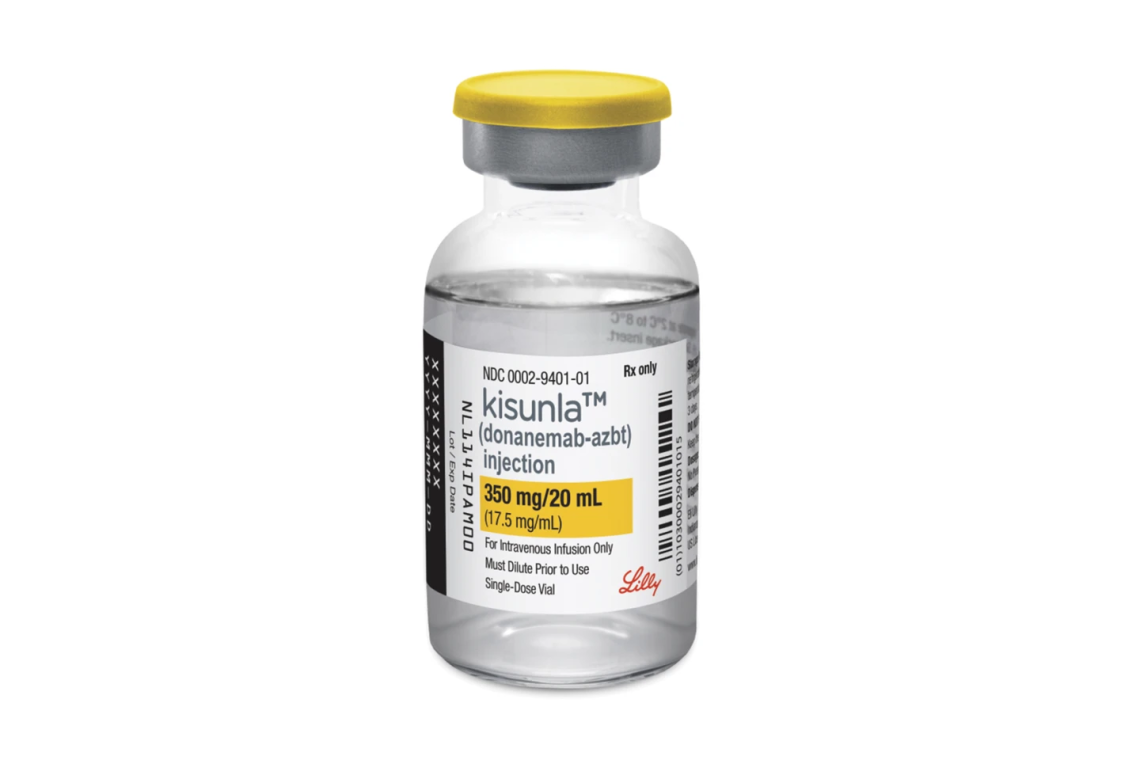
Reporters uncover conflicts and dubious data on latest Alzheimer’s drug
A blockbuster story in The BMJ showed major concerns surrounding the approval process, efficacy and safety of the Alzheimer’s drug…

-
What journalists should know before diving into drug investigations
Learn how two investigative journalists uncovered a trove of information about the recently approved Alzheimer’s drug donanemab.

-
FDA to launch ‘active’ monitoring system to improve medical device safety
The new system aims to detect potential safety issues with medical devices nearly in real time by monitoring data like…

-
What to know about FDA’s new Digital Health Advisory Committee
The administration’s panel on digital health was spurred by the recent explosion of AI in health care, said one committee…

-
FDA wants more data on MDMA therapy for PTSD
The agency’s decision on MDMA-assisted therapy to treat PTSD could be a pivotal moment in psychedelic research and potential legalization.