Tag
Centers for Medicare & Medicaid Services
-
•
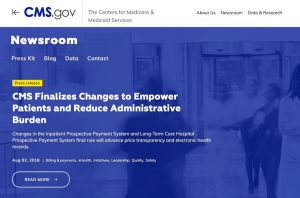
CMS updates website with reporters’ needs in mind
Based on feedback from journalists, the Centers for Medicare & Medicaid Services has updated its online “Newsroom” with the goal…

-
•
CMS threatens to bar Modern Healthcare from press calls after reporter refuses to alter story
The Centers for Medicare & Medicaid Services threatened to ban a reporter from participating in the federal agency’s telephone news…

-
CMS moves into the future, and looks back
As we cover leadership changes at the federal Centers for Medicare and Medicaid Services (CMS), it is worth reflecting on…

-
AHCJ webcast will address how payers, providers are implementing bundled payment
Late last month we wrote about criticism leveled at the federal government’s latest bundled payment proposal. Since then, other experts…

-
Add context to your reporting by recalling who Medicaid actually serves
Here is an article that stood out amid the tidal wave of media coverage of Medicare and Medicaid’s 50th anniversary…

-
•
Reporting team scrutinizes Medicare Advantage
The Center for Public Integrity’s series unearthing potential fraud and waste under the Medicare Advantage program had little help —…

-
•
How to cover nursing homes with more depth and data #ahcj13
It was worth the wait to attend one of the last sessions on the last day of Health Journalism 2013.…

-
Rau explains using data to write about hospital readmissions
Many health policy experts believe that hospital readmissions are symptomatic of the broad dysfunction of the health care system in…

-
•
New tool allows searches of nursing home inspection reports
For the first time, reporters anywhere in the country can search nursing home inspection reports online and see how often…

-
•
Hospital sues to block release of records
Parkland Memorial Hospital in Dallas, the subject of recent reports that patients were at risk, has sued the Texas attorney…