
A new study provides a rare example of something akin to a head-to-head comparison of the quality of care delivered at hospitals run by the Veterans Administration (VA) versus those outside this federal system.
In this case, the advantage appears to go to the VA on a measure of how likely patients were to remain alive within a month of being treated with emergency care.
This study focuses on veterans aged 65 years or older who were enrolled in both the Veterans Health Administration and the Medicare program, reported David C. Chan, M.D., Ph.D., of Stanford University and co-authors in a paper published by the BMJ on Feb. 16. (This paper is available under open-access terms, making it freely accessible to the public.)
Chan and co-authors focused on cases of medical crises involving emergency ambulance rides with lights and sirens that originated from 911 dispatch calls. They used data from the VA, Medicare and Social Security Administration to track what happened to these veterans in the 30 days following these episodes. They also honed in on cases involving veterans who lived within 20 miles of at least one VA hospital and at least one other kind of hospital.
There were 9.32 deaths per 100 patients in those seen at the VA hospitals, Chan and co-authors wrote. They reported a 95% confidence interval range of 9.15 to 9.50 for this figure. (For more on understanding confidence intervals, check the glossary in AHCJ’s medical studies section.) For the veterans taken to other hospitals, Chan and co-authors estimated a rate of 11.67 deaths per 100 patients. They cited a 95% confidence interval range of 11.58 to 11.76 for this group.
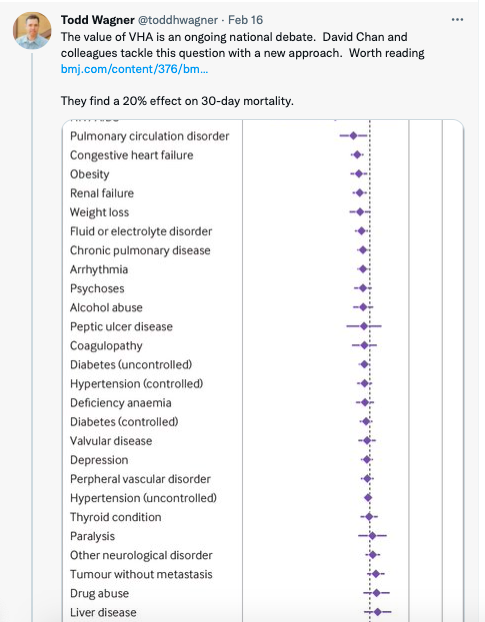
These differences translate into an adjusted mortality rate after 30 days that was 20.1% lower among veterans taken to VA hospitals by ambulances than among veterans taken to other hospitals, Chan and co-authors wrote.
Larger debate on VA health care
There’s been considerable debate for many years about the quality of care provided at the VA.
This intensified around 2012 with many news reports highlighting long wait times for care and some serious missteps by the VA in addressing this concern. In response, Congress working with both the Obama and Trump administrations changed federal law to allow veterans to opt to obtain care in the private sector, Chan and co-authors reported.
“Widely publicized concerns about quality and capacity of the VA system, the largest public healthcare delivery system in the U.S., have fueled public perceptions that the VA health system is falling short of providing good care to the many veterans who depend on it,” Chan and co-authors wrote. “Our findings join those from other studies in suggesting that, for the system overall, those perceptions do not match reality.”
The research presented in the BMJ article was supported by a Veterans Affairs Health Services Research and Development Merit Award (I01 HX002631-01). The VA had “no input in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; or decision to submit the manuscript for publication,” Chan and his co-authors said in the disclosures section.
Chan also reported receiving financial support from a National Institutes of Health Director’s Early Independence Award (1DP5OD019903-01). (There are tips at the end of this article for finding more information about grants such as the ones cited in this article.)
Study design and limitations
The study from Chan and co-authors should interest reporters who cover not only military health issues but those studying comparisons of health systems in general.
The VA has fared well in other comparisons of the quality of care at its hospitals to those in the private sector, but these studies have tended to compare veterans receiving care in the VA health care system with people who are not veterans being seen at other hospitals, Chan and co-authors wrote. They designed their study to compare a similar population of veterans being seen in different settings. They hone in on emergency visits as a way to reduce the potential for self-selection for one kind of hospital or another, they wrote.
“Our primary objective was to obtain a more balanced comparison” of how likely people were to die in the 30 days following emergency care in VA and other hospitals, Chan and co-authors wrote.
And Chan and co-authors reported that the mortality advantage was larger in some groups than for the total population studied:
- For Hispanic patients (22.7% lower; 8.53 deaths per 100 patients taken to VA hospitals v 11.04 deaths per 100 patients taken to non-VA hospitals)
- For black patients (25.8% lower; 7.78 v 10.49)
- Patients aged 65-74 years (27.1% lower: 6.37 v 8.74)
- Patients who arrived with relatively low mortality risk (31.6% lower: 3.91 v 5.72)
Chan and co-authors studied data from cases where veterans were taken by ambulance for emergency care to 140 VA hospitals and 2,622 other hospitals across 46 U.S. states and the District of Columbia in 2001 to 2018.
Chan and co-authors noted that the lower mortality rate for patients taken to the VA hospitals does not persist. At the 15-month mark, the mortality rate for patients taken to VA hospitals had become significantly higher than for those taken to other hospitals. In explaining this finding, Chan and co-authors note that previous studies have suggested veterans who seek out VA care tend to have lower underlying health concerns than veterans who would seek out other hospitals.
Journalists writing about this research should explore this longer-term mortality finding with researchers other than the authors of this study.
In discussing the limitations of their paper, Chan and co-authors noted that their results also might not be generalizable to younger veterans or episodes of care not initiated by emergency treatment.
“Finally, although our results hint at several explanations for how VA hospitals achieved lower mortality rates, the study was not designed to illuminate mechanisms, and we can only speculate on what they could be,” Chan and co-authors wrote.
Still, Chan and his co-authors noted the VA has long provided integrated health care through an advanced information technology system, while other hospitals have struggled to coordinate care this way.
“Other distinctive features of the VA system include organization around primary care, minimal cost-sharing for veterans, and a salaried approach to physician payment that avoids incentives to over-treat or under-treat that are common in private payment models,” they wrote.
Resources
- Chan’s co-authors for the BMJ paper include David Card, Ph.D., of the University of California, Berkeley, and Lowell Taylor, Ph.D., of Carnegie Mellon University. The National Bureau of Economic Research this month also published a working paper by Chan, Card and Taylor, titled, Is There a VA Advantage? Evidence from Dually Eligible Veterans
- For more on waiting time challenges for patients in the VA’s health system, see this 2021 report from the Government Accountability Office (GAO), Priority Open Recommendations: Department of Veterans Affairs. It includes a section on these issues.
- For a deeper look at the concerns about scheduling, there’s also this 2012 GAO report, Reliability of Reported Outpatient Medical Appointment Wait Times and Scheduling Oversight Need Improvement.
Websites on federal health grants
The VA has a website with information about the grants it awards for research on health care. This is a good way to see what the VA is tracking.
A search on the words “emergency care” brings up a list of grants related to this topic, including Chan’s.

Calling up the link for Chan’s grant brings a summary of what he intended to study and why. In it, he notes that the VA has begun to redirect significant resources toward financing care for veterans outside of its own health system, with this policy sometimes called a “make-or-buy” approach.
“However, the quality and cost of care for Veterans that will result from this ‘make-or-buy’ decision remain a scientific unknown, with significant policy implications,” Chan’s abstract for the grant notes. “Quality and cost of care are particularly influenced by emergency services, with 13% of care and more than $800 million in yearly costs directed outside the VA.”
VA grants also appear in the NIH’s RePORTER website for tracking grants. So, if your research isn’t focused on the VA, the NIH site might be a better place to start a search. This is also where journalists can find details on the other grant listed in the BMJ paper, for example, 1DP5OD019903-01 for a project titled The Benefit and Burden of Electronic Reminders for Optimizing Patient Care. You can also see how Chan is listed in the details of this grant and then run a search on his name to see what other grants he has received over the years, as shown here.




