Tag
genetics
-
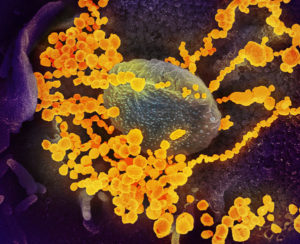
When writing about SARS-CoV-2 variants, utilize metaphors
Writing about how the various COVID-19 vaccines work and the challenges that may lie with emerging genetic variants of SARS-CoV-2…

-
Award-winning genetics reporter shares her process
Sometimes exploring a topic requires more than one story … or three … and sometimes it involves a bit of…

-
Parental life span may foretell a daughter’s healthy aging
Like mother, like daughter? Maybe so when it comes to healthy aging, according to a recent study. Daughters whose birth…

-
Gene therapy development on the rise but costs remain an issue
After decades of unfulfilled promises and setbacks, the field of gene therapy broke through with three FDA-approved products last year,…

-
Researchers identify new genetic stroke risk factors
One of the largest analyses of stroke factors ever conducted is providing scientists with new clues to identify stroke mechanisms…

-
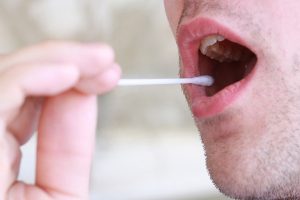
Story about genetic testing company’s problems shows how good reporting stands up to criticism
In December 2016, Charles Piller (@cpiller), the west coast editor for Stat, reported that a genetic test to identify patients…

-
How susceptibility to placebo effect could change research
The placebo effect presents quite the conundrum to researchers attempting to discern whether a particular intervention truly offers clinical benefit…

-
Trade group’s dispute with FDA highlights need to watch for report revisions
The nation’s clinical laboratories have pushed back hard against a proposal by U.S. Food and Drug Administration in October 2014…

-
A problem with precision medicine: It’s not quite precise – at least not yet
At a conference last year, Michael Laposata, M.D., Ph.D., one of the nation’s best known pathologists, explained how clinical laboratories…

-
•
Precision Medicine Initiative: Some quick resources
The White House has announced its anticipated “Precision Medicine Initiative,” which it describes as an “emerging field of medicine that takes into account…