Category
Uncategorized
-
Why deceptive Medicare marketing may impact the health of older adults
We’ve all seen those ads where high-pressure sales tactics are used to encourage older adults to sign up for Medicare…

-
A primer for covering the nursing and hospital battle over mandatory minimum staffing ratios
Nurse staffing ratios are often portrayed as labor disputes; here’s how to cover the patient safety angle.

-
Reporter takes on mental health and caregiving in new documentary
MSNBC reporter and anchor Richard Lui recently debuted his new documentary, Unconditional, which focuses on three families dealing with mental…

-
Why now is the time to report on sepsis
One out of three patients who dies in the hospital has sepsis, which causes 350,000 deaths a year. Here’s how…

-
Tip sheet: Questions to ask at medical conferences when time is short
Here are some of the best questions you should ask presenting researchers, outside experts and attendees at medical research conferences.

-
Why using the term ‘immunity debt’ is problematic for reporters
Photo by Gustavo Fring via pexels.As the number of hospitalized children with influenza, RSV, COVID-19 and other infections continues to soar,…

-
Journalists expose significant problems with Medicare Advantage plans
Seniors signing up for Medicare Advantage (MA) during open enrollment (which ends Dec. 7) have more reasons to worry now…

-
Resources for covering RSV and the ‘tripledemic’
Photo by Andrea Piacquadio via pexels.Are you looking for a Thanksgiving health story? Consider adding the brewing “tripledemic” of pathogens…

-
Experts share databases and other useful resources for U.S. gun violence data
One of the most challenging aspects of writing about gun violence is finding good data. The CDC has reliable statistics…

-
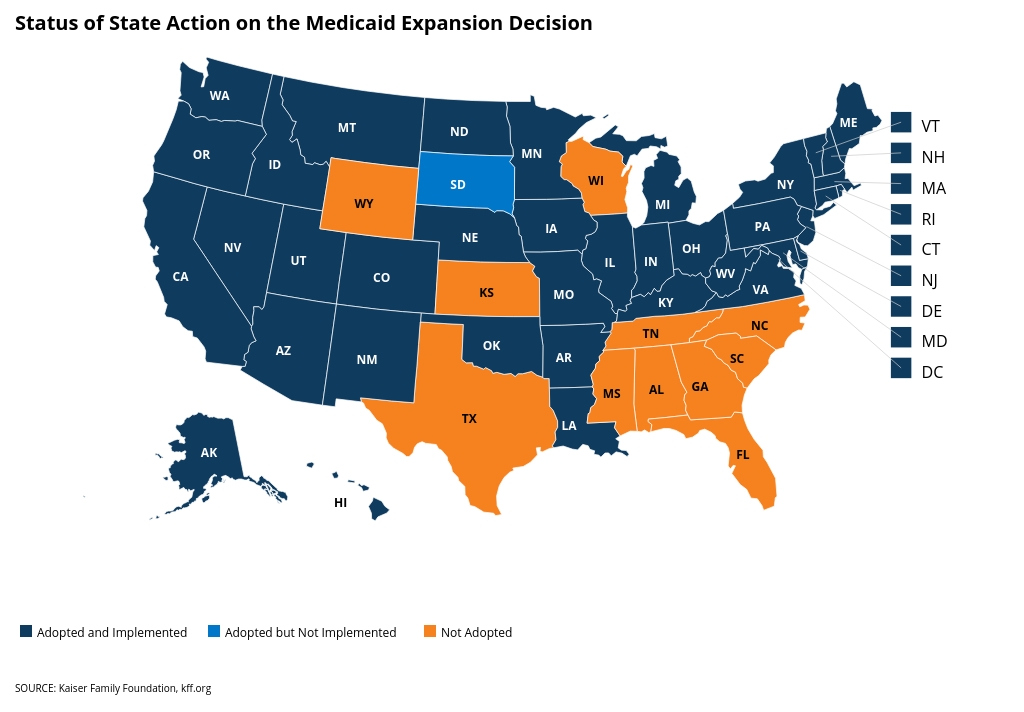
Election coverage lessons on Medicaid expansion, abortion, medical debt and dental insurance
South Dakota voters approve amendment to state constitution to expand access to Medicaid (Source: Status of State Medicaid Expansion Decisions:…