Category
Studies
-
How to prepare to report on a medical research conference
Learn what you should do in the weeks before and during a conference to make for an easier, less hectic…

-
Baby boomers suffer more comorbidities than prior generations at similar ages
Baby boomers may be living longer than their parents or grandparents, but they’re not necessarily healthier than previous generations at…

-
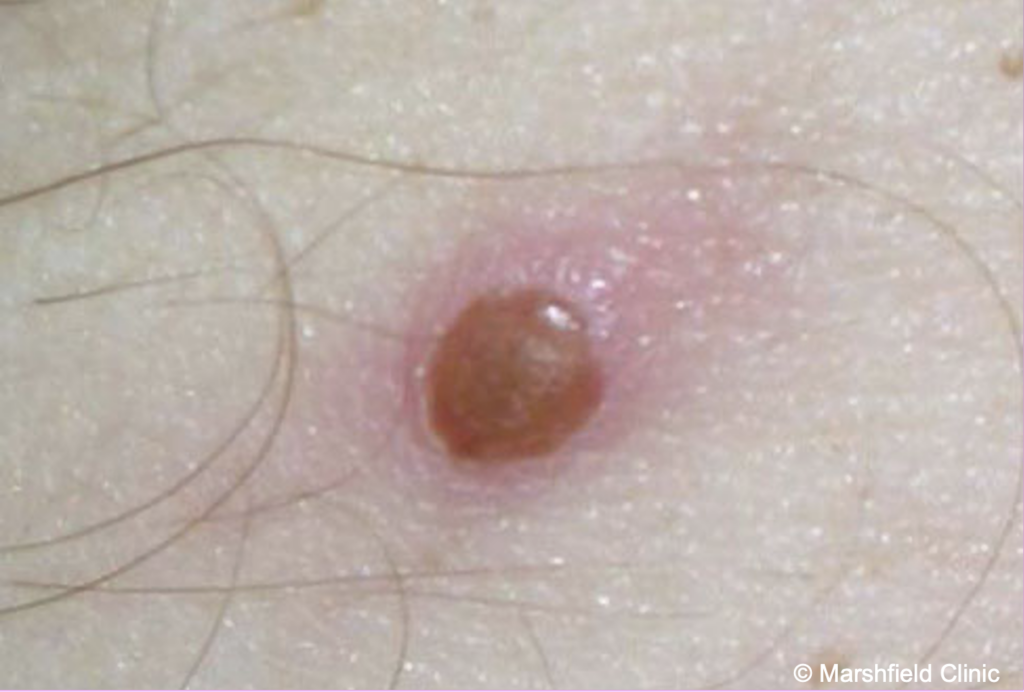
Covering monkeypox: Why imagery matters
The images that accompany health stories can have a significant impact on people’s understanding, attitudes and behaviors regarding a health…

-
White male authors dominate prestigious medical journals
Two of the most influential and esteemed medical journals — if not the top two — are the New England…

-
Mental health disorders soar, but psychiatric bed count remains low
Mental and behavioral health disorders have reached a historic peak. And once again, the nation’s lack of inpatient psychiatric beds…

-
Using Patient Safety Week to report on rising risks
Journalists can use Patient Safety Awareness Week (March 13-19) as an opportunity to question officials at local hospitals and nursing…

-
Falls in older adults on the rise
A new study revealed that despite prevention efforts, falls in older adults have increased by about 1.5% annually, with wide variations in…

-
Understanding statistical bias when covering the use of genomics in medical studies
Rapid advancement in genomics —understanding, identifying and mapping genomes, or the DNA characteristics of a person or a tumor —…

-
•
Study highlights significance of representation in medical school: Why this research matters to reporters
Throughout my reporting of the pandemic, I’ve made an explicit effort to interview many more women than men, especially women…

-
Toolkit offers COVID-19 vaccine story ideas, survey findings on vaccine attitudes
Journalists reporting on the rollout of the COVID-19 vaccine have a new tool to guide their coverage: a Vaccine Education…