Category
Nursing
-
How to the tell the story of nurses of color experiencing racism at work
When Nada Hassanein read the press release about a survey that shed light on racism nurses of color are enduring…

-
Why and how to include more nurses as sources
Patricia Stinchfield, R.N., M.S., C.P.N.P., has just broken a glass ceiling, but it’s probably not the one you’re thinking of.…

-
Health care ballot measures challenge reporters to separate fact from fiction
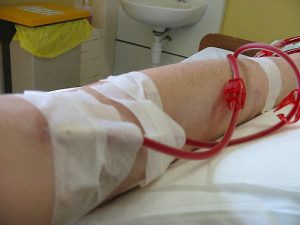
In California, an initiative known as Proposition 8 asks voters to limit the revenue that kidney dialysis clinics can earn.…

-
•
Underrepresentation of nurses in health care coverage continues to be a concern
In 2014, the Ebola outbreak was storming through West Africa and found its way to the United States via four…

-
Stories on changing role of nursing illustrate ‘scope of practice’ issues
On Wednesday, I wrote about “scope of practice” – what health care providers, particularly nurse practitioners, who aren’t physicians are…

-
‘Scope of practice’ stories vary according to state laws
One of the interesting stories to watch in the coming months in the states is the fight over “scope of…

-
•
Investigation reveals N.Y. lax on home care oversight
In the Albany (N.Y.) Times Union, Matt Drange’s investigation is titled “Home health care in crisis.” Having read the piece,…

-
•
American dentistry, a parallel medical universe
NationalJournal’s Margot Sanger-Katz reports on the sometimes woeful state of American dental care, especially for low-income children. And yes, her…

-
•
Reporters spend 10 weeks immersed in end-of-life care
Toronto Globe and Mail reporter Lisa Priest and photographer Moe Doiron spent two-and-a-half months embedded in a 20-bed critical care…

-
Behind Oklahoma’s nation-leading access-to-care problems
In February, the New England Journal of Medicine ranked Oklahoma as the worst when it came to access to medical…