While the Ebola outbreak in the Democratic Republic of Congo was declared over by the World Health Organization in late July, Peter Halfmann, University of Wisconsin Influenza Research Institute associate professor and Ebola researcher, says journalists should keep covering the story in terms of its long-term impact on survivors.
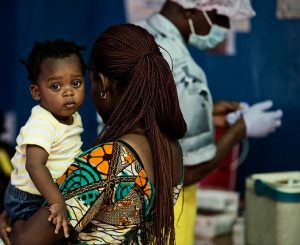
“When the outbreak is over, the story doesn’t end there,” said Halfmann, who spoke during a science webcast sponsored by The Wiley Network, a scientific journal publisher and partner of the Association of Health Care Journalists. “There are 17,000 Ebola survivors so getting those stories is important. They are still suffering.”
On July 24, the DRC declared the end of its ninth reported Ebola outbreak since 1976. There were 54 Ebola cases and 33 deaths. The story of the most recent Ebola outbreak was far different than the one four years ago, when 28,616 people developed Ebola and 11,310 people died, according to the Centers for Disease Control and Prevention.
The west Africa outbreak, which lasted between 2014 through 2016 in three west African countries, cost the world $3.6 billion to fight, reduced the GDP of Guinea, Liberia and Sierra Leone by $2.2 billion and left 17,300 children without one or both parents, according to Halfmann.
“Don’t just focus on the disease alone,” Halfmann urged reporters listening to the webcast. Social factors that contribute to disease and a country’s public health education process are key aspects of the post-outbreak story, he said.
Unlike the situation in the west Africa outbreak, the DRC’s public health community recognized the Ebola cases in the country quickly and global health support swiftly flowed into the country. Further, an experimental vaccine and several experimental treatments were quickly approved under the DRC’s “compassionate use” regulations. None were available in 2014.
About 3,300 people in the DRC were vaccinated, many of them health care workers. Ring vaccination controls outbreaks by vaccinating and monitoring people connected to infected individuals and forming a buffer of immune people to prevent the spread of a disease.
“Great progress has been made in terms of vaccines and understanding the Ebola virus itself,” Halfmann said.
Many unknowns about tackling Ebola still remain.
Recently, researchers found evidence that a female Ebola survivor harbored the virus for more than year and then infected another, suggesting that an outbreak can flare again, long after it is declared over. Further, even though there are now experimental vaccine and treatments, most of these medical measures still aren’t approved by regulators. Scientists had hoped that the DRC outbreak would provide an opportunity to gather more efficacy data, but there turned out to be few Ebola patients to treat.
“There was a scramble to get these different products approved, but they were approved as the outbreak started to end and studies had to end early,” Halfmann said. “So we don’t know what [are] the most effective means to combat Ebola.”
Halfmann added that journalists play an important “middle-man” kind of role in getting information from public health officials to communities and getting information from communities to government officials.
As an example, he cited a radio station in Guinea, that “transformed a forum on [Ebola] into a national forum for public health … and continues to educate the country on public health [topics], which is very important,” he said.
For global health outbreak resources, Halfmann says journalists should turn to the WHO because they usually have staff or bring staff into the country where an outbreak is occurring and they will conduct daily briefings for journalists. He also suggests looking at HealthMap, a free Internet-based information system that visualizes up-to-date reports of disease outbreaks. Another organization that tracks global disease outbreaks is the Global Infectious Disease Epidemiology Network, a subscription-only database that gathers data from government and scientific sources.
For further reading and info: