Tag
prescribing
-
CDC: Update of national antibiotic resistance figures due next month
Since 2013, the U.S. Centers for Disease Control and Prevention has been saying that, in their conservative estimate, at least…

-
Tips for examining the risks, benefits of OTC pain relief
Physicians are being encouraged to curtail prescribing of powerful narcotics in response to the nation’s opioid crisis. So some patients…

-
Reporter tracks medical board investigation into opioid prescribing
What happens when the medical board of a major state begins reviewing fatal opioid overdoses with an eye to disciplining…

-
New poll: More counseling, prescribing limits needed for seniors using opioids
Nearly a third of older adults have received a prescription for an opioid pain medicine in the past two years,…

-
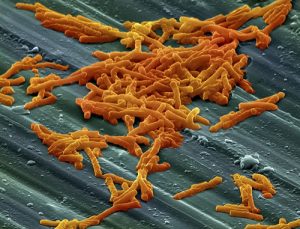
Unnecessary prescribing of dental antibiotics may be adding to C. diff cases
Potentially deadly Clostridium difficile (C. diff), which sickened an estimated half million Americans one recent year, has gained notoriety as…

-
Reporter looks at why, how clinic banned drug reps and their samples
Six years ago, a clinic in Oregon made the decision to ban representatives from the pharmaceutical companies. The doctors and…