Category
Children
-
Addressing childhood abuse could prevent firearm violence later in life
A recent study shows people who experience child abuse are at risk for gun violence perpetrated against themselves and others…

-
Tips for reporting on the ongoing pertussis outbreak
The U.S. is in the midst of the largest outbreak of pertussis (whooping cough) in a decade, and it hasn’t…

-
CDC establishes new reference value for dangerous blood lead levels
The Flint, Michigan water crisis remains a prime example of the importance of public health journalism. Without the dogged reporting…

-
Dallas, Baltimore children’s hospitals embrace high-tech features in behavioral health areas to promote calmness
Children and teenagers presenting to emergency rooms with behavioral health crises sometimes wait hours to days for a bed in…

-
CDC highlights case study on how schools could reopen safely
To showcase how schools could reopen safely this year, Centers for Disease Control and Prevention director Robert Redfield, M.D., highlighted…

-
NEA president to join webcast on re-opening schools
Lily Eskelsen García, president of the National Education Association, will join AHCJ’s webcast, “Reporting on school reopenings in the time…

-
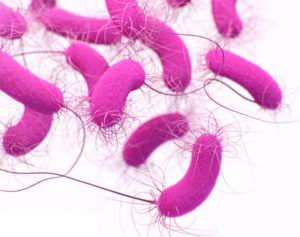
Tips for covering the latest news about antimicrobial resistance
The danger of antibiotic resistance became clearer in November with the release of new figures showing that antibiotic resistance is…

-
Are state bans on vaccine exemptions the right approach?
Is eliminating the religious or philosophical exemption from vaccinations the right public policy tool to stop and prevent measles outbreaks?…

-
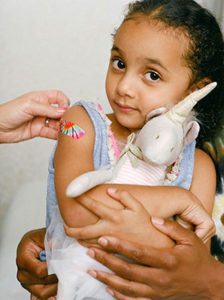
Self, AAP collaborate on library of vaccine images for free use
Photos accompanying news stories about vaccines are notoriously awful, both in effect and in verisimilitude. They often feature large needles…

-
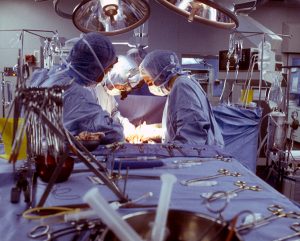
New data resource on NSQIP database can inform coverage of relevant medical studies
More than 1,500 peer-reviewed studies have relied on a surgical database known as the National Surgical Quality Improvement Program (NSQIP),…